The Light at the End of the Tunnel
For millions with treatment-resistant mood disorders, mental health care innovation can’t come quick enough


By Stephen Dark
March 6, 2026
Bob Jeffries* felt he had nowhere to turn.
Diagnosed with depression and ADHD in his teens, the 21-year-old had seen many psychiatrists, taken innumerable medications, and undergone multiple therapies. Nothing worked. “I was torn between my ambition to study medicine and apathy.”
Bob is one of the estimated 5 million Americans who have been diagnosed with treatment-resistant depression.
“Our need for additional innovation is critical,” said Deborah Yurgelun-Todd, PhD, vice chair of research at Huntsman Mental Health Institute at the University of Utah. Antidepressants, one of the last blockbuster mental health medications, debuted in the 1990s. “Thirty years on, we now see that, for some individuals, they display a highly limited effectiveness,” she said. “The field is at an absolute deficit. The scale of our mental health problems is growing faster than we can account for.”
This disconnect leaves people like Bob waiting on the sidelines for a miracle.
Mental health care is painfully slow to advance for many reasons. Central nervous system disorders are notoriously complex, making the development of compounds time-intensive and the results often unpromising. When innovative treatments are developed, they often lack insurance coverage. Patients are required to pay out of pocket, ruling out many potential beneficiaries who can’t afford them.
Where diagnoses of psychiatric conditions like depression are often tied to clusters of symptoms rather than underlying causes, effectively targeting treatments becomes much harder. Many treatments involve significant trial and error, and patients often respond to treatments only partially, if at all.
To understand what innovation in mental health care means, talk to those on the frontline at Huntsman Mental Health Institute—those driven by the same spark of hope that Bob holds in his heart.
In 2025, Daniela Solzbacher, MD, Dr med, was the medical director of the Treatment-Resistant Mood Disorder (TRMD) Clinic at Huntsman Mental Health Institute. TRMD refers to mood disorders, including major depressive disorders, that don’t respond to first-line or second-line treatments.
Solzbacher met with and recommended a treatment to Bob, then brought up a National Institutes of Health-funded second phase trial led by her colleague, clinician-researcher Brian Mickey, MD, PhD.
Run in conjunction with Jan Kubanek, PhD, a former assistant professor in the Department of Biomedical Engineering at the University of Utah, the trial built on the invention of an ultrasound delivery device that showed promising results in treating depression. Bob was so desperate that he was willing to try anything.
Bob Jeffries found his passion for medicine during his service mission for The Church of Jesus Christ of Latter-day Saints. He volunteered at a Midvale clinic, where he saw how access to free health care helped impoverished minority communities.
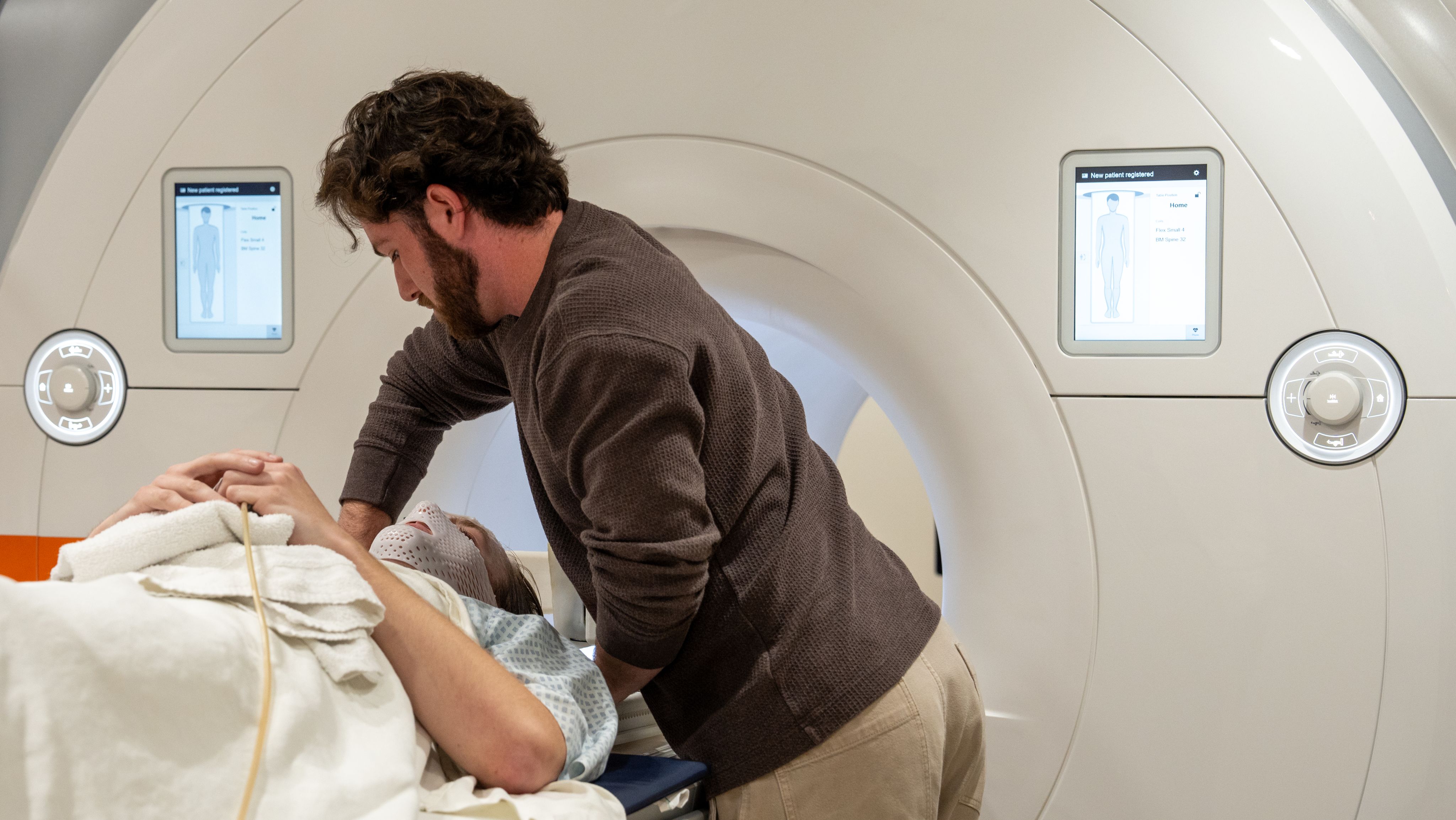
He lay in the MRI machine for 75 minutes. Every 10 minutes, Mickey’s team stimulated different sections of Bob’s brain with five bursts of ultrasound, some real, others not. During two of the five bursts, Bob noticed a buzzing in his ear.
The machine slid him back out, and a smiling Bob sat up. To his astonishment, his depression was gone. How could that be?
By the end of his third treatment, he was happier, more invested in his life. He felt hope.
When Mickey debriefed him after his final treatment, Bob was disappointed. He wanted badly to see what the treatments could do if they continued beyond this trial. Fear mingled with disappointment. What if his depression came back? What if his improvements were only temporary?
He didn’t mention that to Mickey. Instead, he clung to the hope the trial had awakened: “Oh man, this is good. I want more, I want so much more.”
A few weeks after his treatment finished, Bob held on firmly to the hope he’d continue to feel stable. “I've had medications where it’ll work for a little bit, but then it’ll fade away,” he said. “That's the fear I’m dealing with right now.” But even with that fear, his life has changed dramatically. He’s got back into sports and is dating. The thought of living a happy life and getting old had terrified him before. Now, a happy life seems meaningful, beautiful, and obtainable.
A Pressing Need on Our Streets
Brian Mickey’s passion has always been understanding the mysteries behind psychiatric illness and why the brain can malfunction. Following his neuroscience graduate degree, he focused on the brain circuitry that drives happiness, sadness, and pathological emotions. He wanted to know how physicians could intervene therapeutically to modulate activity in the brain pathways and stabilize patients.
What shaped the young resident’s intellectual passion for mental health care innovation was his time at the University of Michigan Hospital, storied for its mood disorder research history. There, Mickey worked with severely ill patients in a catatonic and non-functioning state. He’s never forgotten one patient in her early 70s.
The woman had a long history of bipolar disorder, mood disorders, and numerous hospitalizations. She was admitted after she stopped talking and eating. Diagnosed with dementia, she was put on hospice. Mickey and his colleagues thought her mood disorder history required treating her depression with ECT, the only brain stimulation treatment then available. The day after her first session, Mickey was astounded to find her sitting up and talking with nurses and patients. A few days later, she packed her things to leave and live an independent life. Depression, it turned out, was the cause of her disassociation.
In 2016, what drew Mickey to the University Neuropsychiatric Institute—now Huntsman Mental Health Institute at the University of Utah—was its large clinical population more than willing to participate in research. Interdisciplinary collaborations at the U also piqued his interest. That’s where Jan Kubanek stepped in.
Driving Kubanek was something he saw every day on America’s streets, be it San Francisco, New York, or Salt Lake City: homelessness. Up to one-third of patients with treatment-resistant neurological and mental disorders ended up in a spiral of self-medication, substance abuse disorder, and homelessness.
“There’s got to be something we can do about this,” he thought. “If it’s a disorder of the brain, we need to somehow reset the malfunctioning brain regions.” Such an approach needed to be not only non-invasive but also economically accessible, practical, and scalable.
The answer, he realized, was ultrasound, which had the potential to non-invasively modulate deep brain structures in humans.
There was just one problem: the skull weakened and distorted ultrasound.

“Let’s Do It”
At Stanford University, Jan Kubanek worked on understanding how ultrasound affected brain cells. When he moved to the University of Utah, he planned to develop hardware to deliver ultrasound. In 2018, Kubanek pitched graduate Tom Riis on joining his lab to build the device he had in mind.
Kubanek had already flagged the project to Mickey, who thought it was brilliant. Until then, the only way to selectively reach deep-brain areas was surgically, but that was too invasive for most patients. “We have to do this,” Mickey told Kubanek.
In 2022, Kubanek got back in touch. “Okay, we built it. Let’s test it out.”
What Kubanek and Riis had created, Mickey said, “was a device that measures the distortion of the ultrasound as it’s going through the skull and then corrects for that distortion. By doing that, you can actually deliver ultrasound with a known intensity to a known target deep in the brain.”
Mickey, Kubanek, and Riis designed studies using brain imaging to measure the effects of ultrasound on patients. If they stimulated areas of the brain, what would people experience? Would they notice it happening, or would they notice anything changing? Typically, with non-invasive treatments, change can take weeks. But their device provided surprising news.
The first trial involved patients struggling with depression. The first patient tolerated the treatment well but experienced no significant mood changes.
The second participant had received ECT following a history of treatment-resistant depression, but its initial positive effects were not long-lasting. When the participant arrived, she was in a sour mood. She griped about having dinner with her husband that night.
“She went into the MRI with a very low mood, as if it were dark winter,” Kubanek said. “When she came out, winter had become a bright, summer evening.” She talked excitedly about the dinner with her husband, but now she jovially announced she intended to force-feed him a pickle, which he detested.
Kubanek, Mickey, and Riis were astonished. They had not anticipated such rapid change. In retrospect, Kubanek notes, since the ultrasound was modulating deep brain structure, it made sense the effects were quick.
The next day, the patient told Mickey she hadn’t felt this good in three years. “It feels like my brain has been woken up.” Her positive response lasted for over a month.
A Question of Time
By the end of the first trial, several participants demonstrated rapid and long-lasting improvement in depression. That’s what the researchers needed to attempt a trial conclusively demonstrating long-lasting relief from major depressive disorders. “That gave us the fortitude to push through and make it into a longer study,” Mickey said.
But while some experienced changes lasting for months, others lasted only hours. “It does seem to vary, and we don’t know why,” he said.
The researchers received NIH funding for the second-phase trial, focused on understanding how patients respond to different levels of stimulation and how specific the effects are relative to the stimulation’s focus.
Once a large-scale phase 3 clinical study has been conducted—Riis said a trial for chronic pain is starting this year—then they will seek FDA approval. The targeted reset of the brain has a good future, Riis notes, especially once they develop a wearable device. “We’re excited to move on to the next stage, get FDA approval and then out to society. It’s about making it happen.”
For research participants like Bob Jeffries, taking part in trials to support mental health care innovation is bittersweet, given there’s no idea when the treatments might become publicly available.

Daniela Solzbacher MD, Dr med, was driven to paint out of necessity. She sees it as a “powerful tool to create an opening and direct experience of the present moment.”
Daniela Solzbacher, MD, Dr med, was driven to paint out of necessity. She sees painting as a “powerful tool to create an opening and direct experience of the present moment.”
Rediscovering Joy
Daniela Solzbacher came to psychiatry like someone rediscovering a forgotten friend. As a student in Germany, she intended to pursue psychiatry, but her interest in surgical procedures led her to become an ENT surgeon. Visiting Salt Lake City 10 years later, local psychiatrists convinced her to return to her first love. She completed additional training at the University of Utah and joined Lowry Bushnell, MD, who, in the 1990s, founded the Electroconvulsive Therapy (ECT)/Neuro-stimulation Service.
ECT uses electric stimulation to induce a therapeutic seizure, long known to alleviate or even resolve short- and long-term mental health issues, particularly depression.
Contemporary ECT therapy is honed to target and impact the body. The patient is placed under general anesthesia and muscle relaxant, then given a few seconds-long controlled electrical charge via electrodes placed on the head. The patient’s hand or foot is isolated from the rest of the body by a pressure cuff, stopping the muscle relaxant from reaching it. Through the clenched fist’s movements, the physician can monitor the length of the seizure.
Bushnell was a passionate believer in electroconvulsive therapy (ECT). He was a national pioneer in inviting patients’ loved ones to witness ECT treatments to demystify and destigmatize a practice long tainted by brutal media portrayals.
With a 70-90% effectiveness in treating depression, “ECT is the gold standard service for severe and refractory illness,” Solzbacher said. That’s particularly true when it comes to patients who have battled treatment-resistant mood disorders for decades and who have no more options—like Cody Harris.
Daniela Solzbacher was driven to paint out of necessity. She sees painting as a “powerful tool to create an opening and direct experience of the present moment.”
Daniela Solzbacher was driven to paint out of necessity. She sees painting as a “powerful tool to create an opening and direct experience of the present moment.”
Rediscovering Joy
Daniela Solzbacher came to psychiatry like someone rediscovering a forgotten friend. As a student in Germany, she intended to pursue psychiatry, but her interest in surgical procedures led her to become an ENT surgeon. Visiting Salt Lake City 10 years later, local psychiatrists convinced her to return to her first love. She completed additional training at the University of Utah and joined Lowry Bushnell, MD, who, in the 1990s, founded the Electroconvulsive Therapy (ECT)/Neuro-stimulation Service.
ECT uses electric stimulation to induce a therapeutic seizure, long known to alleviate or even resolve short- and long-term mental health issues, particularly depression.
Contemporary ECT therapy is honed to target and impact the body. The patient is placed under general anesthesia and muscle relaxant, then given a few seconds-long controlled electrical charge via electrodes placed on the head. The patient’s hand or foot is isolated from the rest of the body by a pressure cuff, stopping the muscle relaxant from reaching it. Through the clenched fist’s movements, the physician can monitor the length of the seizure.
Bushnell was a passionate believer in electroconvulsive therapy (ECT). He was a national pioneer in inviting patients’ loved ones to witness ECT treatments to demystify and destigmatize a practice long tainted by brutal media portrayals.
With a 70-90% effectiveness in treating depression, “ECT is the gold standard service for severe and refractory illness,” Solzbacher said. That’s particularly true when it comes to patients who have battled treatment-resistant mood disorders for decades and who have no more options—like Cody Harris.
On the surface, 36-year-old Cody had it all: a loving wife, two young daughters, and a well-paying job he enjoyed. Privately, it was a different story. Diagnosed with depression at age 6, Cody attempted suicide several times by 18. He went through hundreds of doctor-prescribed medications and numerous therapists. Every time that he found a drug to manage his OCD, anxiety, and depression, it would eventually stop working.
At family dinners, he’d wear noise-cancelling headphones and his beanie. When he got home, he went to bed, covered himself in a weighted blanket, and didn’t move.
“All you could see was pain,” his wife Lisa said. “There was no joy in his countenance.”
On the day of his oldest daughter’s church baptism, he was so paralyzed by anxiety that only his father could calm him down. Hospitalized shortly afterward, he told his therapist and the attending doctor, “Things have to change or I’m going to die. This is my life.”
But a week later, when Lisa drove Cody to the clinic at 7:30 am for his first ECT session, he had no faith it would work. “I want to go to sleep and not wake up,” he thought.
Solzbacher encouraged Lisa to sit in the operating room for the treatments.
“We're trying to change the narrative of ECT,” Solzbacher told her. “We encourage family involvement to gain understanding and advocacy for this treatment.”
Each session, Solzbacher asked Cody, “How are you feeling? Do you notice any improvement?”
Cody was too exhausted to notice anything, but Lisa could see improvements. His countenance changed drastically. Gone were the dark circles around his eyes as he finally slept. He went to family dinners without headphones or beanie.
At one dinner, she heard him make a strange sound. “That was a genuine laugh,” she thought, overwhelmed by emotion.

Eventually, they tapered down sessions to twice a week, then once a week, and finally only when needed. Their oldest daughter, Tessa, marveled at the change. “Dad used to come home and go straight to bed. Now he comes home and plays with me.”
Lisa has struggled to trust that her “second husband”—as they jokingly refer to Cody now—is there for good. Part of her worries that the old Cody may one day return.
Cody cannot believe the new him either. “I’ve never felt total joy like I’ve felt this last year. I can close my eyes and it’s dark and quiet. It’s unreal. I love it.”
So Close, Yet So Far Away
If Lowry Bushnell was a pioneer of inviting friends and families to witness ECT to combat its negative image, colleagues say Daniela Solzbacher has been equally innovative. As medical director, Solzbacher increased patient numbers at the TRMD Clinic and doubled the treatment rooms for electric convulsive therapy. The clinic also evolved to support innovation.
Benjamin Lewis, MD, an inpatient psychiatrist and clinician-researcher at Huntsman Mental Health Institute, credits Solzbacher with developing the clinic as a central support hub for innovation at the institute.
“A whole clinic focused on treatment-resistant mood disorders with a number of different kinds of treatments available, including ECT, Transcranial Magnetic Stimulation, and ketamine, is innovative,” Lewis says. Such a comprehensive approach represents a “robust model uncommon even in academic centers.”
The clinic monitors their patient intake and queries to identify potential recruits for innovative research trials.
“We're really the only clinic in Utah that offers the entire bandwidth plus all these cutting-edge research developments,” Solzbacher said.
Resetting the Brain
What inspired Benjamin Lewis, MD, to pursue innovation in mental health care was a growing sense of unease with his own profession. As a psychiatrist, Lewis primarily treats severely and persistently mentally ill patients, so many of the problems he and other psychiatrists deal with stem from deeply entrenched, systemic societal problems. This is not to say that inpatient psychiatry does not do a lot of good, he stresses—it very much does. But the intersection of severe mental illness with an infrastructure that offers few (if any) treatments often generates feelings of inadequacy in providers, who fret at their inability to help patients move toward more stable lives.
Alongside Paul Thielking, MD, then a psycho-oncologist at Huntsman Cancer Institute and one of his teachers during residency, Lewis became fascinated by psychedelics’ potential to treat depression. To date, early phase trials had demonstrated promising, significant, and sustained therapeutic changes, even following a single dosing session.
Psilocybin, the active ingredient in so-called “magic mushrooms,” is a compound that acts on the serotonin system in the brain, has wide effects across brain networks, and induces significant acute changes in consciousness. Psilocybin works on network-level functioning in the brain, resulting in more flexible neurotransmission: the brain is temporarily “freed up,” opening up a window for change. This is particularly significant for mental health conditions characterized by rigid or repetitive pathways or patterns.
“There’s less constraint on neural network activity and crosstalk, and you can reset how different networks function,” Lewis adds. This renders the brain more flexible. New ways of thinking and behavioral patterns become possible for patients. However, this is not a safe treatment for every mental health condition and is not recommended in the context of risk of psychosis or mania. Even apart from these conditions, there are risks associated with psilocybin and other psychedelic drugs, given the significant changes to consciousness and associated sensitivity to environmental factors.
In 2018, Lewis and Thielking decided to run a pilot study of psilocybin-assisted group therapy for cancer patients. There was a big learning curve ahead, dealing with a Schedule 1 drug and navigating the FDA, the DEA, and U of U Health’s own IRB. COVID-19 slowed the initiative, but when the pandemic wound down, Lewis and his team got a Schedule 1 license and launched their first foray into psychedelic research—the aptly named HOPE trial.
Clinical trial participant Laura Tripp, who received counseling, meditation, and a new purpose in her life.
Clinical trial participant Laura Tripp, who received counseling, meditation, and a new purpose in her life.
My Friend the Mountain
The HOPE trial was the first modern trial to employ a full group model. Previous psilocybin trials have employed an individual format with two therapists present for each participant. While increasing the scalability of this intervention, the group model also simultaneously encourages interpersonal connection and shared experience: factors recognized to be important in depression.
The trial involved 12 cancer patients who engaged with the study in groups of four. Prior to the seven-hour group “dosing day,” there were three two-hour group therapy sessions. Then, following the dosing day, participants completed three group sessions to integrate into their lives what they had learned about themselves, their individual experiences, and the collective experience of the group.
Laura Tripp was in the first group of the HOPE trial. After her 2021 diagnosis of a rare form of Stage 1 breast cancer, she underwent chemotherapy, which accentuated her depression and filled her with rage at no longer being able to pick up her children, who were 2 and 4 years old. At the back of her mind were questions over what would happen to them if she died. Midway through her chemo, she learned of the HOPE trial and signed up.
Each participant was paired with a therapist who accompanied them through the trial. During preparatory sessions, in-depth discussions explored themes related to illness and death, dying and depression.
Laura talked to the other female patient, who had Stage 4 cancer. They got to know each other during the study and often took walks together outside of the study-related processes (as well as after the study was completed). This friendship changed Laura’s life.
Dosing day fell on Halloween 2021. It took place in a Huntsman Cancer Institute infusion suite. Lewis and his colleagues decorated it with tapestries and flowers and tried to make it as comfortable and non-medical-appearing as possible. Speakers were used to play a seven-hour music playlist.
After the initial check-in, the participants shared their intentions for the day. Several hoped to feel better and function better. Laura wanted to lose her fear of death. Her friend had not set intentions.
They gathered in a circle, took their psilocybin capsule, and lay down. After six hours, the effects started to wear off. When they regrouped, some were talkative, others were quietly processing.
While Laura’s own experience felt significant, she was deeply impacted by the experience of her friend, who described her body becoming a mountain, down to the rock and dirt. Laura said her friend became “my mountain, a towering strength who could not die, even as she showed so much grace navigating her own death.”
According to Lewis, the study revealed a pronounced effect on depressive symptoms sustained to six months with a single dosing session.
Laura discovered through the trial not only the healing power of meditation, which helped her find peace from her chaotic life, but that she had a core set of values she wanted back.
Before cancer, Laura had been a corporate engineer in Salt Lake City. She suffered from imposter syndrome and felt she was fading out of her life. But after the trial, she wanted to do something she felt passionate about, where she was doing good for people. She and her husband, a pharmacist, bought a small-town pharmacy in Sutherlin, Oregon, in June 2023. Her husband ran it, and a year later, she and their children joined him.
As president of Sutherlin Drug, Laura loves running her own Main Street business, hanging flower baskets outside, delivering medications, and, as the Chamber Ambassador director, promoting her hometown. Her husband jokes that they’re “small-town famous.”
Looking back, Laura got so much from the HOPE trial. “I learned to use my life to the best potential that I can. I am still scared to die—I’m terrified. But I got all the counseling, I got meditation, and I got a new purpose: I wasn't going to accept a passionless life.”
Lewis, too, found answers. HOPE brought him back to the roots of why he went into medicine in the first place: to help people. “Somehow, I’d allowed myself to lose contact with that.”
My Friend the Mountain
The HOPE trial was the first modern trial to employ a full group model. Previous psilocybin trials have employed an individual format with two therapists present for each participant. While increasing the scalability of this intervention, the group model also simultaneously encourages interpersonal connection and shared experience: factors recognized to be important in depression.
The trial involved 12 cancer patients who engaged with the study in groups of four. Prior to the seven-hour group “dosing day,” there were three two-hour group therapy sessions. Then, following the dosing day, participants completed three group sessions to integrate into their lives what they had learned about themselves, their individual experiences, and the collective experience of the group.
Laura Tripp was in the first group of the HOPE trial. After her 2021 diagnosis of a rare form of Stage 1 breast cancer, she underwent chemotherapy, which accentuated her depression and filled her with rage at no longer being able to pick up her children, who were 2 and 4 years old. At the back of her mind were questions over what would happen to them if she died. Midway through her chemo, she learned of the HOPE trial and signed up.
Clinical trial participant Laura Tripp, who received counseling, meditation, and a new purpose in her life.
Clinical trial participant Laura Tripp, who received counseling, meditation, and a new purpose in her life.
Each participant was paired with a therapist who accompanied them through the trial. During preparatory sessions, in-depth discussions explored themes related to illness and death, dying and depression.
Laura talked to the other female patient, who had Stage 4 cancer. They got to know each other during the study and often took walks together outside of the study-related processes (as well as after the study was completed). This friendship changed Laura’s life.
Dosing day fell on Halloween 2021. It took place in a Huntsman Cancer Institute infusion suite. Lewis and his colleagues decorated it with tapestries and flowers and tried to make it as comfortable and non-medical-appearing as possible. Speakers were used to play a seven-hour music playlist.
After the initial check-in, the participants shared their intentions for the day. Several hoped to feel better and function better. Laura wanted to lose her fear of death. Her friend had not set intentions.
They gathered in a circle, took their psilocybin capsule, and lay down. After six hours, the effects started to wear off. When they regrouped, some were talkative, others were quietly processing.
While Laura’s own experience felt significant, she was deeply impacted by the experience of her friend, who described her body becoming a mountain, down to the rock and dirt. Laura said her friend became “my mountain, a towering strength who could not die, even as she showed so much grace navigating her own death.”
According to Lewis, the study revealed a pronounced effect on depressive symptoms sustained to six months with a single dosing session.
Laura discovered through the trial not only the healing power of meditation, which helped her find peace from her chaotic life, but that she had a core set of values she wanted back.
Before cancer, Laura had been a corporate engineer in Salt Lake City. She suffered from imposter syndrome and felt she was fading out of her life. But after the trial, she wanted to do something she felt passionate about, where she was doing good for people. She and her husband, a pharmacist, bought a small-town pharmacy in Sutherlin, Oregon, in June 2023. Her husband ran it, and a year later, she and their children joined him.
As president of Sutherlin Drug, she loves running her own Main Street business, hanging flower baskets outside, delivering medications, and, as the Chamber Ambassador director, promoting her hometown. Her husband jokes that they’re “small-town famous.”
Looking back, Laura got so much from the HOPE trial. “I learned to use my life to the best potential that I can. I am still scared to die—I’m terrified. But I got all the counseling, I got meditation, and I got a new purpose: I wasn't going to accept a passionless life.”
Lewis, too, found answers. HOPE brought him back to the roots of why he went into medicine in the first place: to help people. “Somehow, I’d allowed myself to lose contact with that.”
The Loneliness of the COVID-19 Provider
For the next psychedelic project, Benjamin Lewis focused on burned-out health care providers. The PAPR trial was named after the acronym for the respirators doctors and nurses wore while treating COVID-19 patients. Lewis and his co-investigator, John Hendrick, MD, developed a study combining mindfulness training and a group psilocybin intervention for health care providers dealing with COVID-19-related depression and burnout. All participants completed an eight-week Mindfulness-Based Stress Reduction (MBSR) course, and half of them were randomized to also partake in a group psilocybin session at six weeks.
Selecting participants, Lewis was shocked by the levels of stress and distress his peers displayed, among them an emergency medicine physician, Sarah.*
Through her life, Sarah had taken hard times in stride, whether it was her mother passing away when she was 17 or confronting the physical and emotional extremes of ballet as a professional dancer in the Atlanta Ballet. As an adjunct faculty member at University of Utah Health, Sarah couldn’t understand anyone feeling suicidal. “None of that made sense to me.”
But then the pandemic brought the world to a halt, and she fell apart. Shortly after the birth of their third child, Sarah’s husband lost his job. She felt constantly miserable and sad, convinced she wasn’t a good mother. She didn’t sleep, she lost weight, and she struggled with the antidepressants her primary care physician prescribed. Two colleagues took their own lives. Sarah thought, “I get it.”
She was teetering on the edge of collapse. “It was like a puzzle I couldn’t solve.”
When she heard about the PAPR trial, she wasn’t convinced psilocybin was a good idea. Would it pull away what little was holding her together? But after her screening visit for the study and learning about the trial, she put aside her skepticism and fear of psychedelics and thought,
“I can do this.”
Sarah was convinced that if she meditated daily per the trial’s requirement, she could get herself out of her depression. By Dosing Day, she felt she was better but pressed on anyway.
With three fellow participants in her group, she showed up at Huntsman Mental Health Institute at 7:30 am. Walking into the institute was hard. It was an acknowledgment she belonged there, she thought—that she was “off.”
The room’s windows offered a panorama of the valley and the snow-dappled Oquirrh Mountains beneath a majestic gray sky. After a 10-minute seated meditation in a circle, Sarah took her psilocybin capsule and lay down on her mat, with therapist Amanda Stoeckel, PhD, sitting next to her. Sarah chanted the mantra she and Stoeckel had decided on: “In and through.”
Sarah felt the effects come on quickly—it felt like the medicine was coursing through her body, as if she were being scanned.
She felt in her experience as if she ran through the clouds for 7,000 years. She introduced her deceased mother to the grandson she had never met. She walked with humanity, from the first person to the last. Love swelled and rushed through her.
And then guilt set in. It was a weekend—and dinner time. She should be home with her kids.
She looked up at Stoeckel. “I can't do this.”
“In and through,” Stoeckel said. “In and through.”
Looking back, Sarah realized during the dosing session that she had a sense of connecting with her best self—the person she wanted to be from then on. When she got home, she kissed each of her children, the most wonderful experience in the world.
Over subsequent months, she changed.
As an ER doc, she had simply endured emotionally challenging situations. Now, she acknowledges pain and provides meaningful comfort. She feels more durable as a provider. She told her husband, “If you take your defenses down, you can see what’s actually there—and then you can deal with it.”
Most of all, Sarah has become the parent she knows she always was but had lost sight of through her depression and struggles. Her journey—and other participants’ journeys—with psilocybin humbled Lewis. “You’re not delivering some treatment that’s just going to fix people,” he said. “You’re offering a pathway that they can use how they choose.”
Sarah revisits her journey often, the PAPR playlist on her earbuds as she runs along the Wasatch Front, flowing through the clouds.
Healing Reimagined
While pursuing these clinical trials, Benjamin Lewis had nursed the idea of opening a Ketamine-Assisted Psychotherapy (KAP) Clinic. If taken in sub-anesthetic doses under medical supervision, ketamine has significant promise for treating depression and anxiety.
While the institute’s TRMD clinic had been offering ketamine via infusions, Lewis wanted to try a different approach and pursue a way of working with ketamine that incorporated a robust psychotherapeutic intervention. He pursued specialized training with the vision to build a clinical program that could accommodate emerging psychedelic medicines upon FDA approval and become a hub for clinical care, research, and training/education.
In January 2023, Lewis opened the institute’s Ketamine-Assisted Psychotherapy (KAP) Clinic in Park City, treating patients with depression and anxiety, cancer and end-of-life distress, and PTSD. It also helps those seeking an accelerant for intensive psychotherapeutic work on their depression and anxiety. The KAP Clinic has since moved from Park City to the Huntsman Mental Health Institute Crisis Care Center to increase patient access to this treatment.
What Lewis loves about the clinic is that it’s a team effort. The team includes two MDs and four therapists who are passionate about the work, the therapeutic approach, and the vision for a more holistic and healing approach to psychiatric care.

“When There’s Nothing Else, There’s Love”
One patient who wanted to benefit from that acceleration was Suzy Mang. In 2020, she was diagnosed with a rare incurable cancer—gastrointestinal stromal tumor—for which she had been taking grueling daily targeted chemo. It left her with intense, demanding side effects, including explosive GI distress, brain fog, muscle cramps, and persistent depression.
She wanted to sign up for HOPE, but the trial was full. So instead, she opted for ketamine-assisted psychotherapy, even though she knew being unemployed with limited health insurance would make the $500 session a hardship. She drew on funds a friend had loaned her.
Her therapist was Cristie Frey, LCSW, who, Suzy said, “held a non-judgmental, loving open space” for her to prep for the medicine-assisted psychotherapy.
Clinical trial participant Suzy Mang, embracing a personal goal to complete the El Camino trail.
Clinical trial participant Suzy Mang, embracing a personal goal to complete the El Camino trail.
Suzy’s mind fought the ketamine tooth and nail during the first session. After some disassociation, she found herself asking, “What is this? Why are you doing this?” Lewis and Frey said some minds don’t want interference. Suzy persisted.
Her third ketamine session was emotionally powerful. “I felt a vortex of love that was orange, pink, and yellow, with my daughters, their partners, and my animals swirling about in a funnel of love.”
A fourth session brought similar feelings to the third, while the fifth felt dense and dark—like an immobile void.
The final session brought it all together. Suzy experienced light, density, and beauty accompanied by astonishing music. “It just sang into my soul,” she said. “It made me vibrate. I was singing along, I was crying.” Frey marveled at how Suzy hummed and swayed, as if in a ceremony, all the while smiling in tears.
For Suzy, Frey and Lewis were lifesavers. “They made me see things with new eyes,” she said. She gave them a gift. As she stood up, she smiled at them and said, “When there's nothing else, there’s love.”
“We'll hold onto that one for a long time,” Frey thought.
Healing Our Society
While Daniela Solzbacher, Brian Mickey, Benjamin Lewis, and others collaborate on numerous projects, the hunger for innovation in mental health care requires a commitment to collaboration on a scale yet unseen. “Innovation has seen very small incremental changes in improving outcomes,” Deborah Yurgelun-Todd said. “We need to do something more dramatic.”
Yurgelun-Todd has spearheaded the idea and construction of a five-floor building in University of Utah’s Research Park that promises a bold future for innovation in mental health care. The Translational Research Building (TRB), which opens in 2027, will challenge institute researchers, scientists, and clinicians to collaborate and innovate like never before to answer the prayers of patients like Bob Jeffries and millions of others.
Yurgelun-Todd is a nationally lauded pioneer at the nexus of mental health and brain research. She has invested a good deal of her life’s learning, research experience, and educational ambitions in the TRB, soon to be home to the only 7-Tesla magnetic resonance imaging scanner dedicated to mental health in the Mountain West. This technology will offer researchers measures of brain metabolism and high-resolution images of the brain in a depth of detail never seen before, providing unprecedented opportunities for understanding brain changes in mental health.
Research psychiatrists Deborah Yurgelun‑Todd, PhD, and Rana Jawish, MD, during their first tour of the Translational Research Building construction site.
Research psychiatrists Deborah Yurgelun‑Todd, PhD, and Rana Jawish, MD, during their first tour of the Translational Research Building construction site.
It mimics the brain’s specialized technical spaces that serve the whole body. The imaging center, pharmacy, freezer farm, auditorium, and café serve the whole building. Just like the brain, every aspect of the TRB has been designed to facilitate collaboration, with hallways, conference rooms, offices, and open spaces all featuring connection points for informal interactions, idea generation, and conversation.
The TRB is designed to shift snail-pace innovation into the highest gear. Crucial to this is overcoming the traditional siloing of mental health research and clinical care, along with the tunnel vision among mental health professionals locked into their own disciplines. “Rather than drawing boundaries around who can contribute, we want to bring them all together,” Yurgelun-Todd said. “No one discipline, be it physiologic aspects of neuroscience, sociodemographic factors, or another side of research, is identified as the most important.”
Rana Jawish, MD, assistant professor in the Department of Psychiatry at the U, embodies the high-energy focus on multi-disciplinary research that Yurgelun-Todd is aiming for.
Complex diseases like addiction need more than one specialty to address them, Jawish notes. Solutions require a team of experts from different disciplines. She works at the intersection of obstetrics and gynecology, psychiatry, neuromodulation, and addiction to realize her vision of developing a new therapy for pregnant women affected by substance use disorder.
For Jawish, the TRB’s confluence of multidisciplinary researchers will provide the perfect environment, infrastructure, and technology needed “for a vision like mine, which thrives in a collaborative environment.”
“The TRB will provide an environment to further advance and evaluate new approaches to mental health treatment, including digital health tools, brain stimulation techniques, novel medications, and psychotherapeutic methods, among others.”
In an era when mental health crises seem ever-more visible and yet treatments seem ever-more limited, Yurgelun-Todd believes the TRB is a turning point in how we approach, understand, research, and investigate mental health. “This is a chance to start to catch up with where we should have been.”
This new building represents a commitment to unify society with those who have mental health conditions at its heart—instead of on its streets.
“It's an embrace of them and their future,” Yurgelun-Todd said.

* These names are pseudonyms to protect the identity of those involved
The Light at the End of the Tunnel
Story by Stephen Dark
Illustrations by Dung Hoang
Photography by Kristan Jacobsen, Laura Tripp, Suzy Mang
Edited by Nick McGregor, Tanner Telford, Jesse Colby
Designed by Geldona Lapi
Produced by Patricia Kingston-Brandt






