The Dirt in Their Veins
FOR MORE THAN A DECADE, RESIDENTS OF A FORMER FUNDAMENTALIST MORMON STRONGHOLD HAD NO ACCESS TO HEALTH CARE. DRIVEN BY THE DIRE NEED IN THEIR REMOTE COMMUNITY, LOCAL LEADERS FOUGHT TO OPEN A CLINIC.

WHEN RICHARD BENNETT WENT TO HIGH SCHOOL IN HANSEN, IDAHO, HIS FARMER PARENTS DID ALL THEY COULD TO PROVIDE FOR THEIR SIX SONS. THEIR LIMITED FAMILY BUDGET MEANT THEIR EVER-GROWING BOYS WORE EACH OTHER’S HAND-ME-DOWNS AND THOSE OF THEIR COUSINS.
Every year, the Bennetts bought each of their children new shoes at an annual $5 shoe sale, an event akin to Christmas for their offspring. There was a catch. One shoe was bigger than the other: the store was willing to sell them cheaply since they didn’t have the pair of either. While Bennett dreaded going to school with mismatched shoes, to his relief, nobody noticed.
In a seemingly forgotten rural town where Main Street concluded with the sign “Dead End,” the only thing Hansen’s largely impoverished, marginalized residents had going for them, Bennett thought growing up, was each other. His parents—and grandparents who lived next door—always tried to help others, sharing what little they had with those in need.
For a family like his, which struggled to afford even gasoline, the nearest hospital being 10 miles away drew a line in the sand. “It had to be serious before Mom would load us into the car and drive us to town,” he says.
Richard Bennett, far right, with his Uncle Jim and four of his six brothers in rural Idaho. His uncle was almost blind and had to walk into town close to 10 miles away for any supplies he needed. His death from a heart attack when Bennett was young is a key reason why he remains dedicated to improving access to rural health care.
Richard Bennett, far right, with his Uncle Jim and four of his six brothers in rural Idaho. His uncle was almost blind and had to walk into town close to 10 miles away for any supplies he needed. His death from a heart attack when Bennett was young is a key reason why he remains dedicated to improving access to rural health care.
THAT REALITY WAS ON BENNETT’S MIND IN THE SUMMER OF 2017, WHEN HE WAS HIRED BY UNIVERSITY OF UTAH HEALTH TO OPEN THE FIRST SATELLITE OFFICE OF THEIR PHYSICIAN ASSISTANT (PA) STUDIES PROGRAM IN ST. GEORGE, UTAH. THE UTAH PHYSICIAN ASSISTANT PROGRAM (UPAP) CELEBRATED ITS 50TH ANNIVERSARY IN 2021, CONTINUING ITS MISSION TO EXTEND UTAH PROVIDERS’ REACH TO AREAS OF MUCH NEED AND NEGLECT.
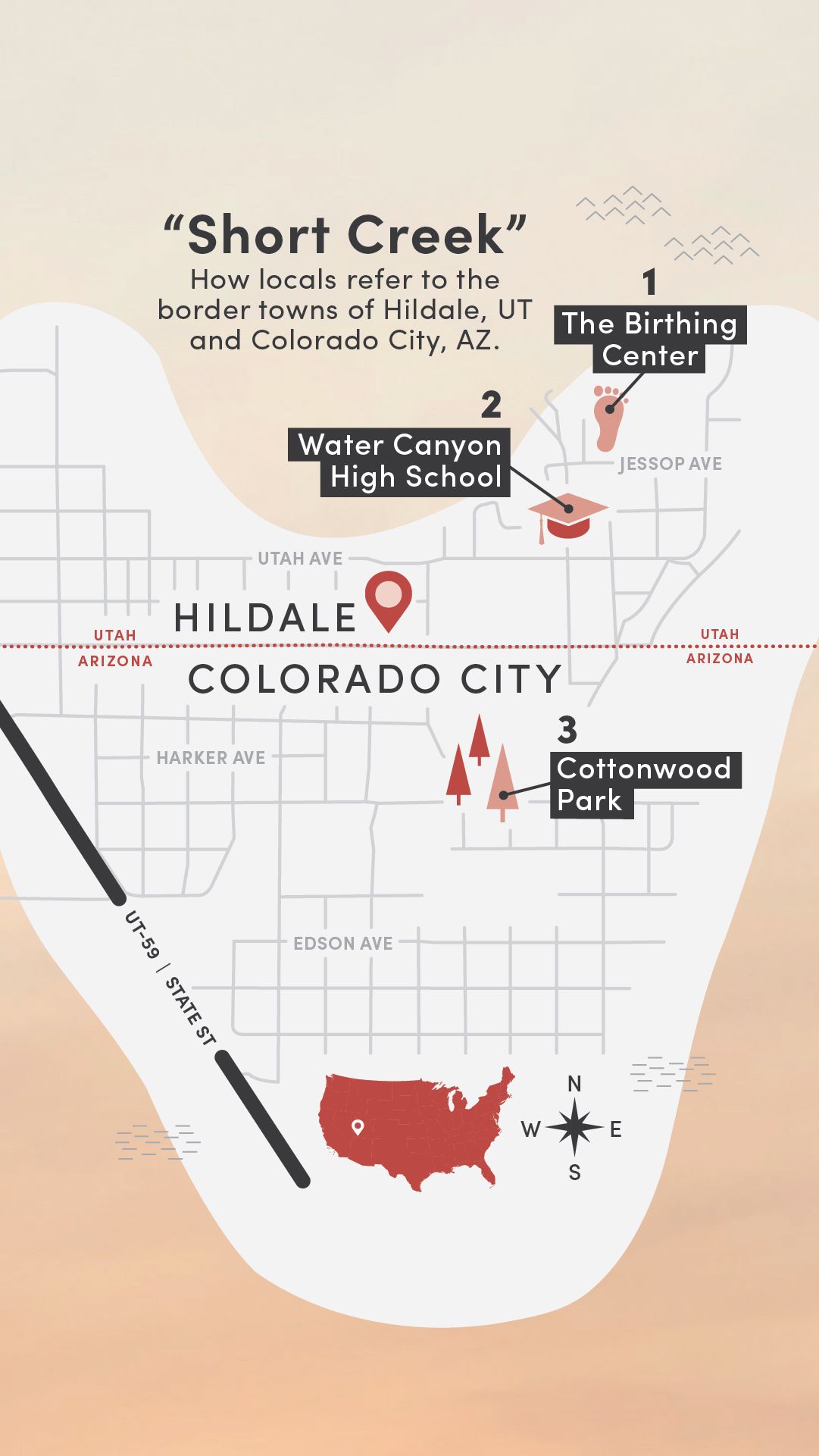
When Bennett asked Washington County’s leaders where the greatest need for services was, they told him Hildale, Utah, and Colorado City, Arizona—neighboring towns on the Utah-Arizona border so close geographically that locals bestowed a single name: Short Creek.
Cradled by the craggy, red-rock Vermillion Cliffs, Short Creek is 30 minutes from clinics in Hurricane, 50 minutes from hospitals in St. George, and an hour from health care in Arizona. It had been more than 10 years since health care was easily accessible in Short Creek.
By the time Bennett arrived, it was hard to imagine somewhere more in need, with close to half the community living below the poverty line.

YET THAT NEED WAS GEOGRAPHICALLY INVISIBLE TO THE REST OF THE STATE, AN INVISIBILITY EXACERBATED BY ITS DEEPLY CONTROVERSIAL HISTORY AS HOME TO THE FUNDAMENTALIST CHURCH OF JESUS CHRIST OF LATTER-DAY SAINTS (FLDS). THE FLDS PRACTICE A RELIGIOUS DOCTRINE KNOWN AS PLURAL MARRIAGE, OR POLYGAMY.
Bennett looked at a Community Health Needs Assessment by Intermountain Healthcare and one prepared by Short Creek-based plural family services’ provider Cherish Families that used federal statistics and local knowledge to delve even deeper into the health problems plaguing the community. They painted a devastating portrait of medical neglect, with diabetes, hypertension, heart disease, and many other chronic diseases running rampant in Short Creek—particularly among women and children. It was also a community plagued by suicides.
When Bennett drove 50 minutes from St. George to Short Creek to see for himself, the 8,000-person-strong twin townships reminded him of his hometown. Just like in Hansen, the streets were mostly dirt paths without curbing or gutters. He’d seen poverty on his LDS mission in Indiana and subsequently during a PA rotation in Appalachia, but nothing that felt so close to home. “How can this be happening under my nose?” he asked himself.
As he talked to locals, he discovered there had long been a push to open a clinic, but it had been stymied by many challenges, including the thorny question of how to fund it. Bennett’s eventual contribution to the efforts—co-organizing two health fairs in 2018 and 2019—may have seemed limited. But the impact of the fairs injected momentum and credibility at crucial moments, boosting the efforts of local providers and community activists to bring health care back to Short Creek.
Jordan Merrill, community health program manager in southern Utah with Intermountain Healthcare, credits Bennett and U of U Health with opening a dialogue of trust between community members, providers, and PA students—many of whom are outsiders. Like Bennett and so many involved in this struggle in Short Creek, Merrill grew up with limited access to health care in Enterprise, Utah, a small rural community. It taught him “that the underserved need to be served as much as anybody else,” he says.
Bennett and Merrill both understood that humility was the only way into the community. That philosophy is driven by the land they came from, a philosophy that joins them to so many others in this story who played more central roles in the evolution of Short Creek’s first independent clinic. What unites them all is the ties that bind—the roots of the past that draw you back—feelings that Bennett knows so well.
At the end of Bennett’s first visit to Short Creek, he felt an ache inside, almost a physical yearning to help the local people. He traced it back to the community in Hansen that had made him who he was.
“The dirt from the farm gets into your veins,” Bennett says. “It gives you this need to give back.”

Homegrown Health Care

AFTER THE CHURCH OF JESUS CHRIST OF LATTER-DAY SAINTS ABANDONED PLURAL MARRIAGE IN 1890, SOME MEMBERS OF THE SALT LAKE CITY-HEADQUARTERED CHURCH CONTINUED THE BANNED PRACTICE BEHIND CLOSED DOORS. ONE BREAKAWAY GROUP OF MORMON FUNDAMENTALISTS, AS THEY BECAME KNOWN, SETTLED IN 1930 ON THE UTAH-ARIZONA BORDER.
They placed land they bought into a trust called the United Effort Plan. Everyone gathered to build a house overnight when needed, in what amounted to communal living and ownership.
A raid on Short Creek by Arizona state officials in 1953 sought to dismantle a town built on plural marriage, the men imprisoned and the women and children sent away. The raid backfired as public sympathy favored the families torn apart by the law. It made the FLDS church more insular, its only connection with the outside a labor base largely made up of construction workers traveling through southern Utah to work. “You’d just be a construction worker as long as your body allows it,” says Tyler Steed, local businessman, part-time teacher, and one of the community activists committed to opening a clinic.
The community grew to around 9,000 people strong at its peak through mostly peaceful years, and health care evolved in the Creek much like everything else did: homegrown, most noticeably a reliance on essential oils, local plants and herbs, and homeopathy.
That homegrown emphasis also extended to those who staffed the main health care clinic in Hildale, Utah, known as the “birthing center.” It was run by “Aunt Lydia” Jessop, who delivered thousands of babies there until her death in 1996. FLDS Church member Norma Richter gave birth to 10 of her 11 children there. “She became the whole community’s mother,” Richter says.
In the 1980s, the fundamentalist Mormon community split in half. What became known as the FLDS remained in Hildale and Colorado City. A breakaway group called Centennial Park established a new community across the Arizona state line in Mohave County. While residents who were not members of the FLDS could still receive care at the Hildale clinic, the welcome they received was increasingly chilly. Centennial set up its own labor and delivery clinic.
After Warren Jeffs became the FLDS prophet in 2002, an autocratic regime ruled over Short Creek, with high walls and metal fences surrounding homes. That included the birthing clinic, as access to health care became increasingly restricted. First outsiders and apostates—the label given to former members by the FLDS—were excluded, followed by those deemed unworthy within the faith, until finally the clinic closed in 2011.
After the arrest of Jeffs and his eventual life imprisonment for child sexual assault, the FLDS community went through a lengthy period of fragmentation. That made the battle to bring medical care to the community more challenging—and more necessary.
The Weight of Trauma

FEW WERE AS AWARE OF THE DESPERATE NEED FOR A HEALTH CLINIC AS AARON KNUDSON. A PHYSICIAN AT BANNER HEALTH IN PAGE, ARIZONA, HE GREW UP IN SHORT CREEK. “IT WAS STORY AFTER STORY AFTER STORY,” HE SAYS, REMEMBERING ONE INDIVIDUAL DIAGNOSED WITH A TERMINAL CANCER FOR WHOM THERE WERE NO TREATMENT OPTIONS, OR ANOTHER ADMITTED TO THE HOSPITAL DUE TO A CONDITION THAT COULD HAVE BEEN MANAGED IN A CLINIC PREVENTING HOSPITALIZATION. “EVERY TIME WE TURNED AROUND, YOU SAW HOW THE NEED WAS SO GREAT—AND JUST SO UNMET.”
Knudson was medical director of a Banner Health mobile clinic that went to Short Creek one day a week in the late 2010s. He and other providers who had grown up in the Creek and studied medicine wanted to see a full-time clinic, but there was no money to support such an initiative. “We explored multiple options,” Knudson says—without success. He knew without a doubt that any clinic had to be staffed by people who understood the local culture. His vision was a clinic that would be akin to Switzerland: neutral and open to all.
If Short Creek’s residents were raised to view outsiders with grave suspicion, when they sought medical help, they were often met with suspicion and judgment themselves. Some residents drove two hours to Page, Arizona, to see Knudson and other providers who grew up in Short Creek. They knew they would receive treatment rather than judgement or prying questions about their faith and personal lives.
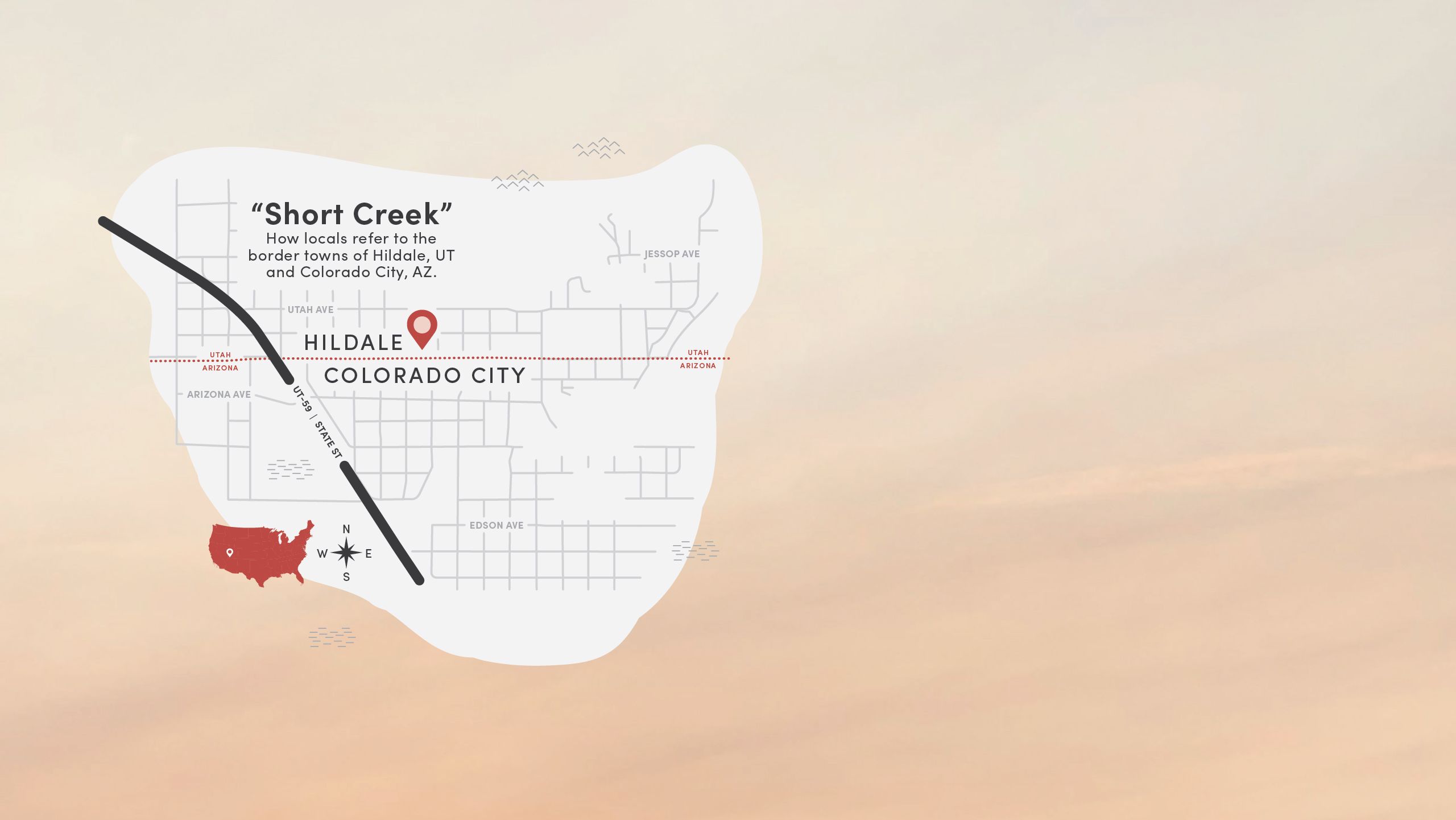
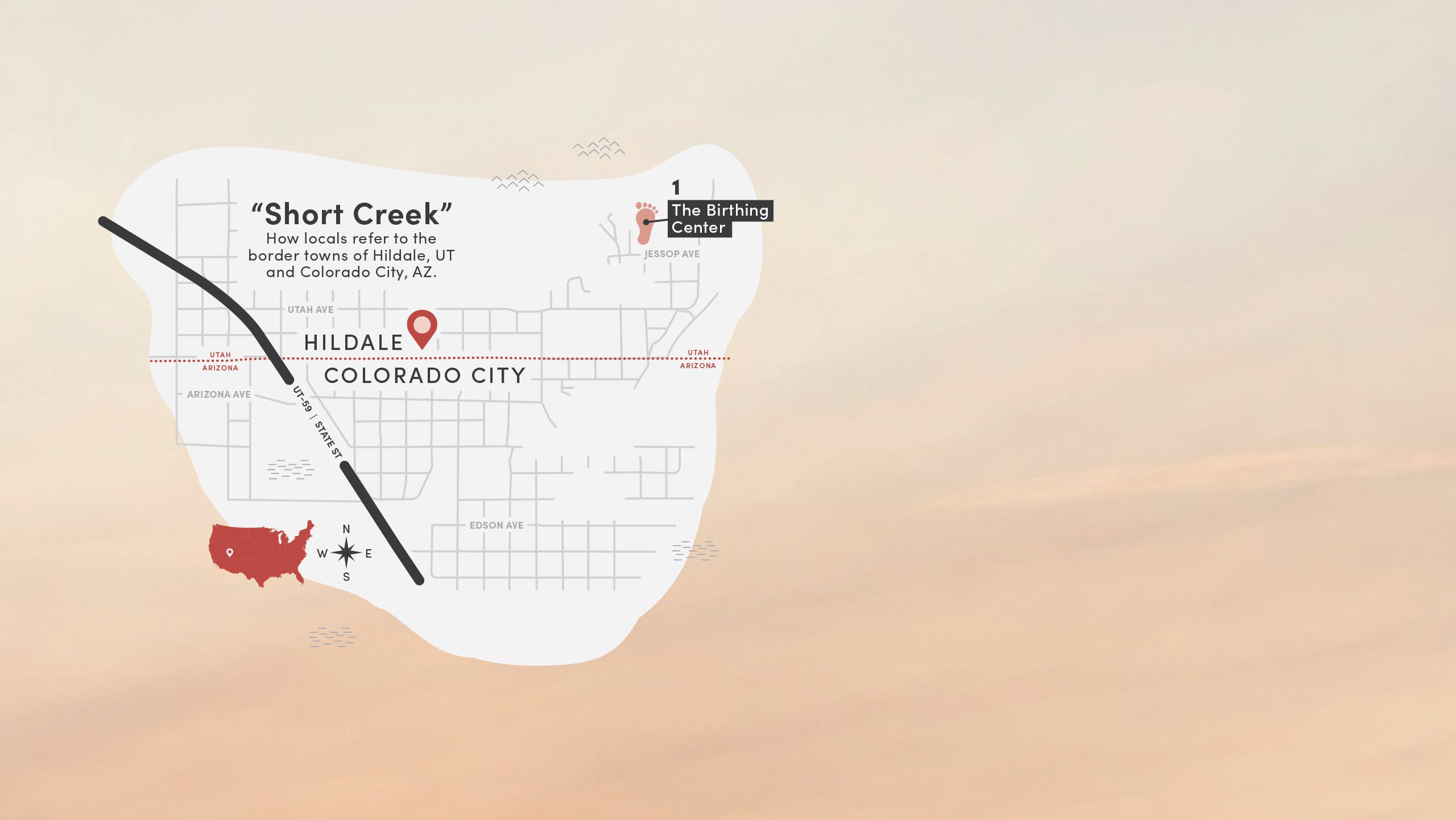
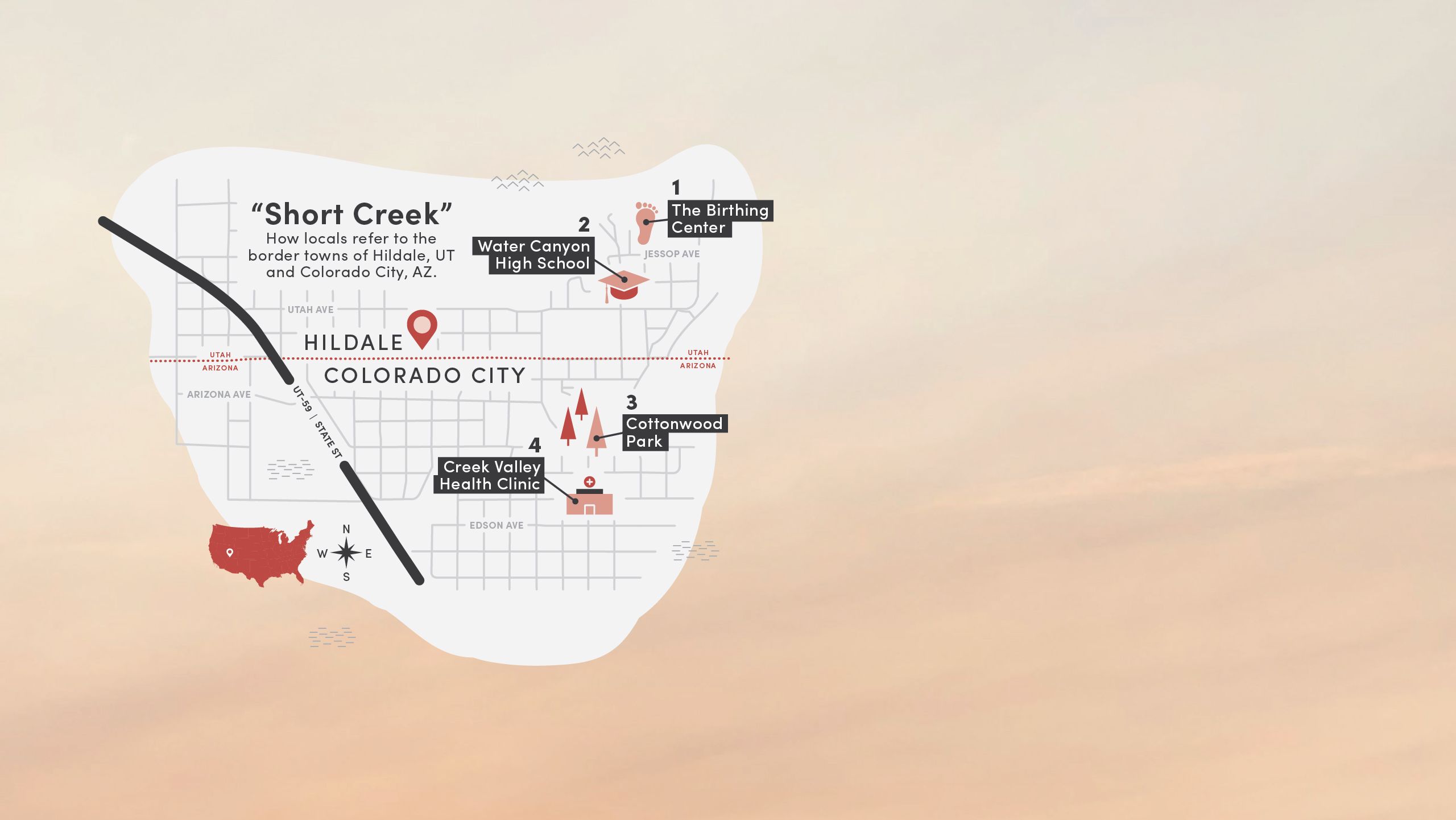
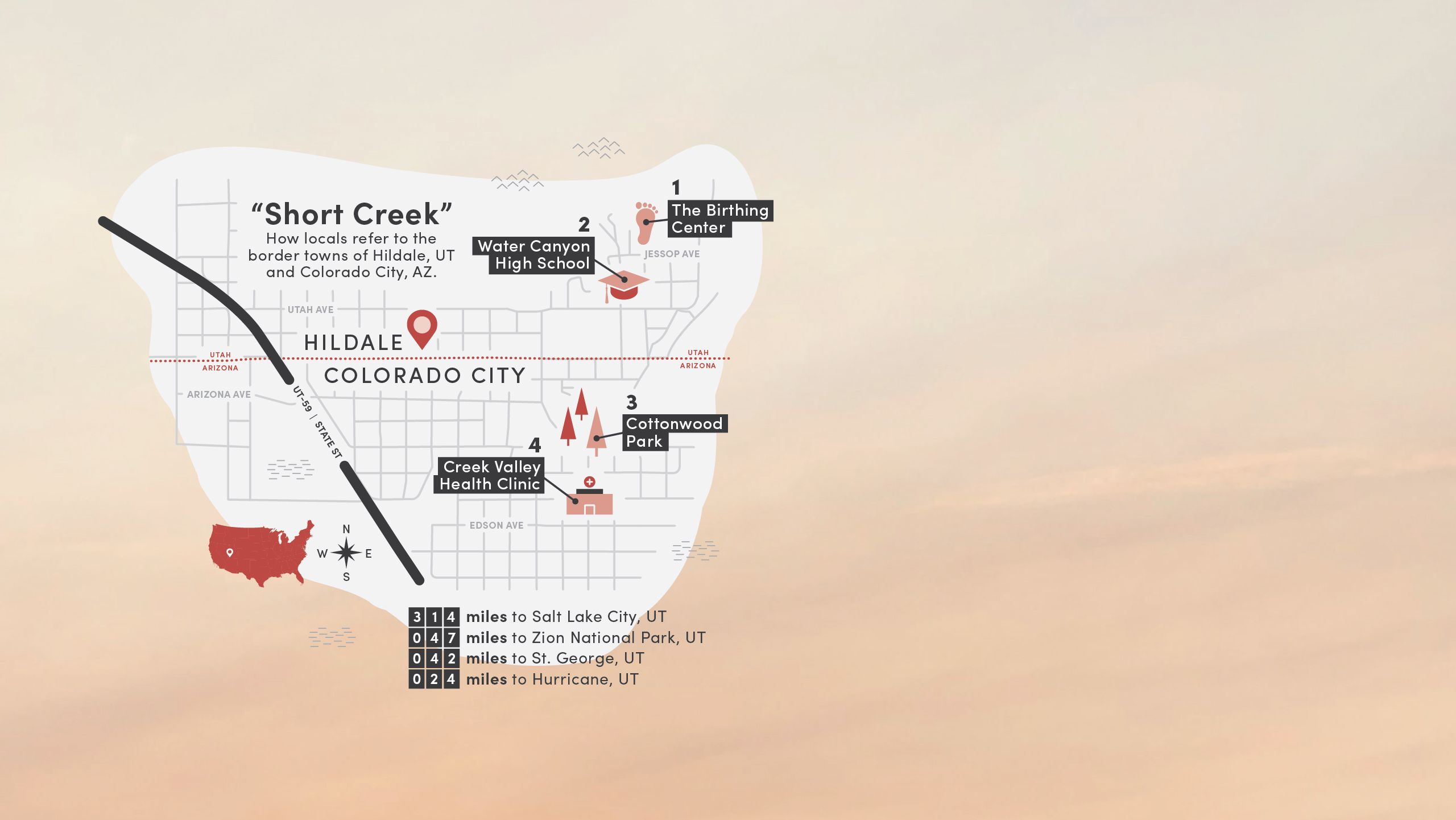
1. The Birthing Center
Historically, the main clinic in Hildale, Utah, was known locally as the birthing center. “Aunt Lydia” Jessop delivered thousands of babies there until her death in 1996. After Warren Jeffs became prophet in 2002, access to health care became increasingly restricted.
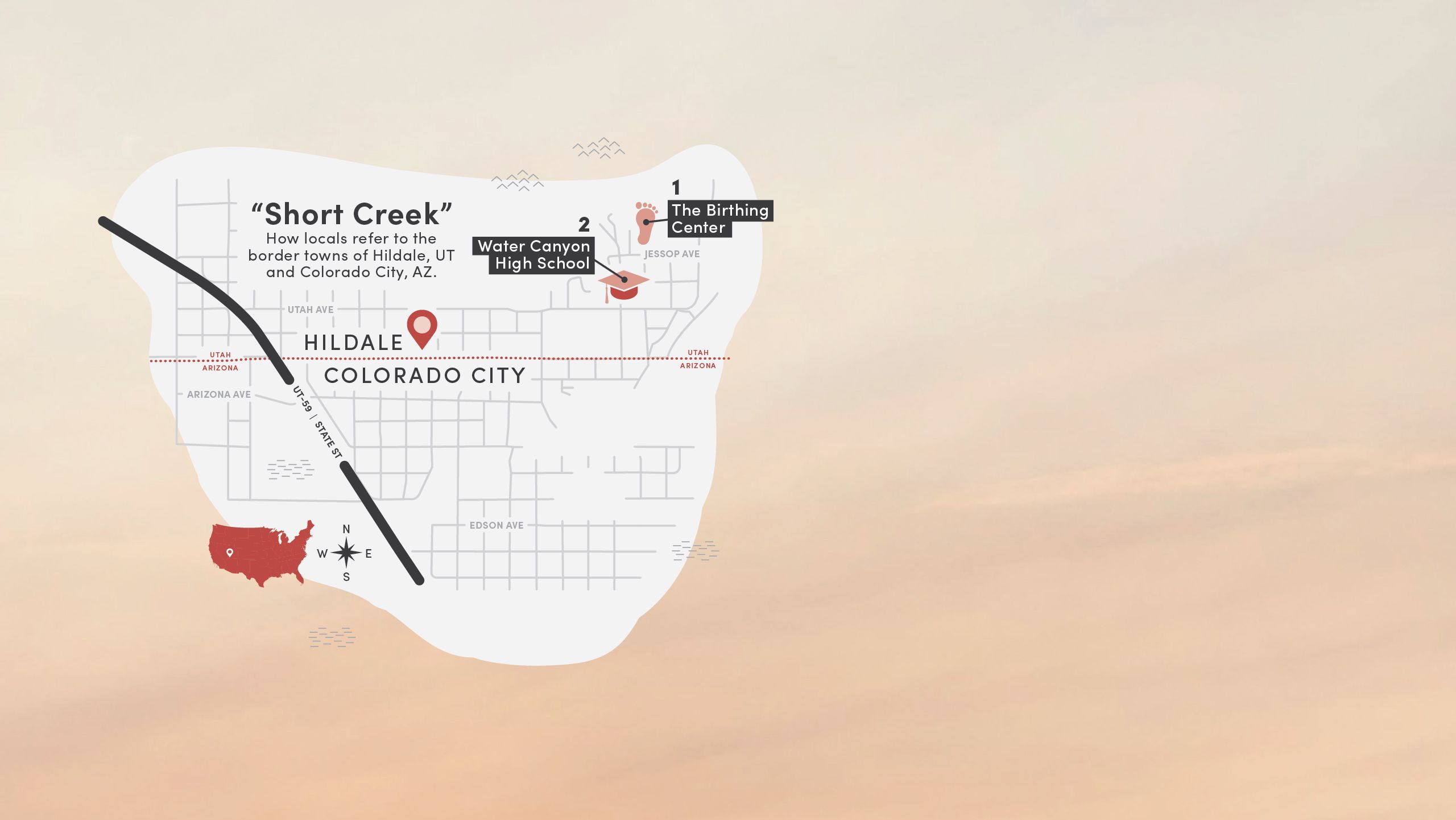
2. Water Canyon High School
The high school agreed to host the health fair in its gym, with the locker rooms available for physicals. Bennett, Draper, and Merrill invited service providers to man booths, and a group of first-year U of U Health PA students signed up to help just weeks into their courses.
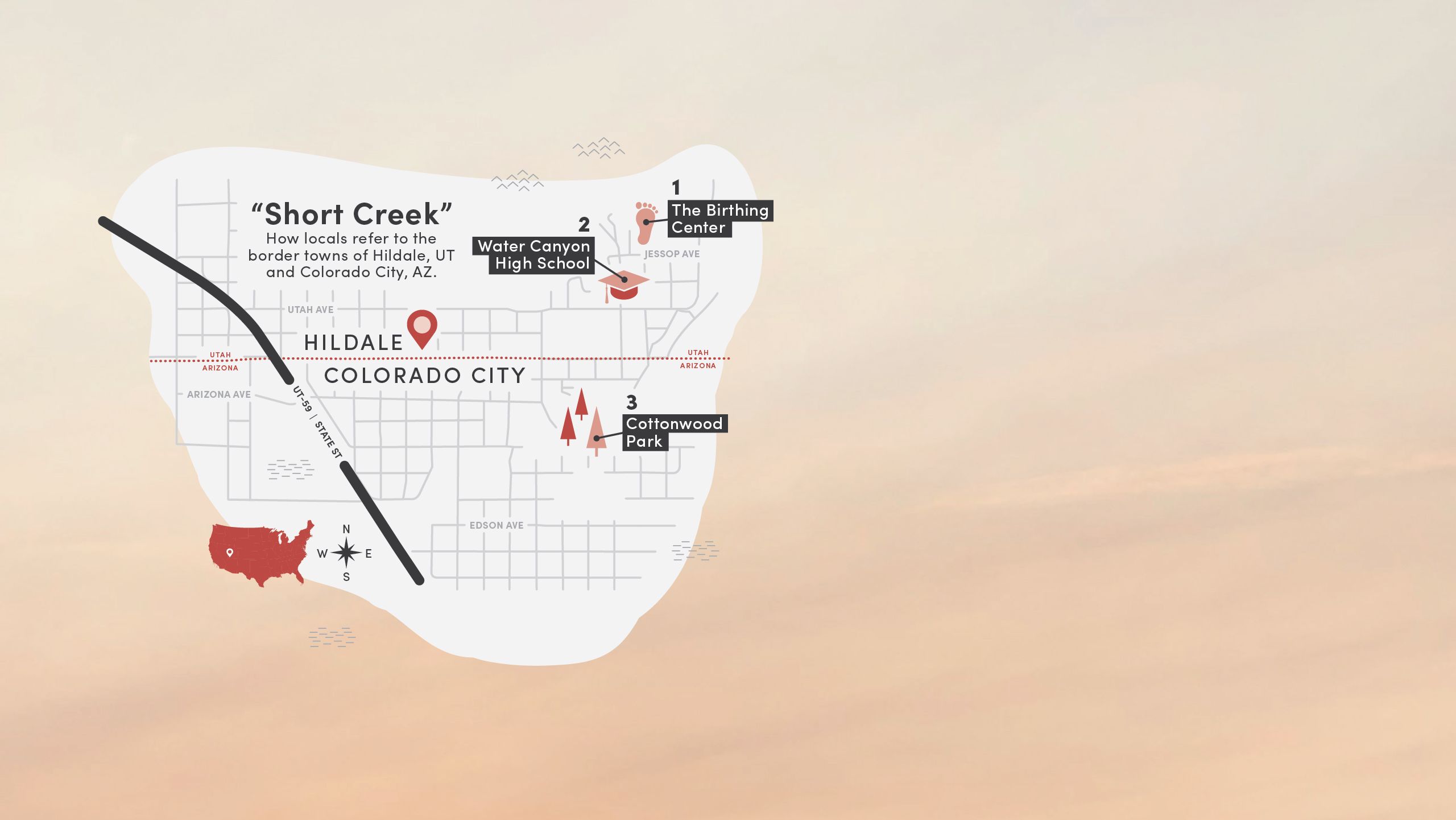
3. Cottonwood Park
Long a place for celebration and gathering for communal parties and parades, Cottonwood Park fell into disuse in the 2000s. In 2018, the park was renovated with fresh sod and a playground and now stands as a flagship for municipal and community efforts to rebuild the Creek.
4. Creek Valley Health Clinic
Incorporated in December 2018, Creek Valley Health Clinic was the brainchild of Steed, Draper and Knudson, among others who championed the idea of opening a clinic with staff and a board drawn from the community who understood its unique needs and history.

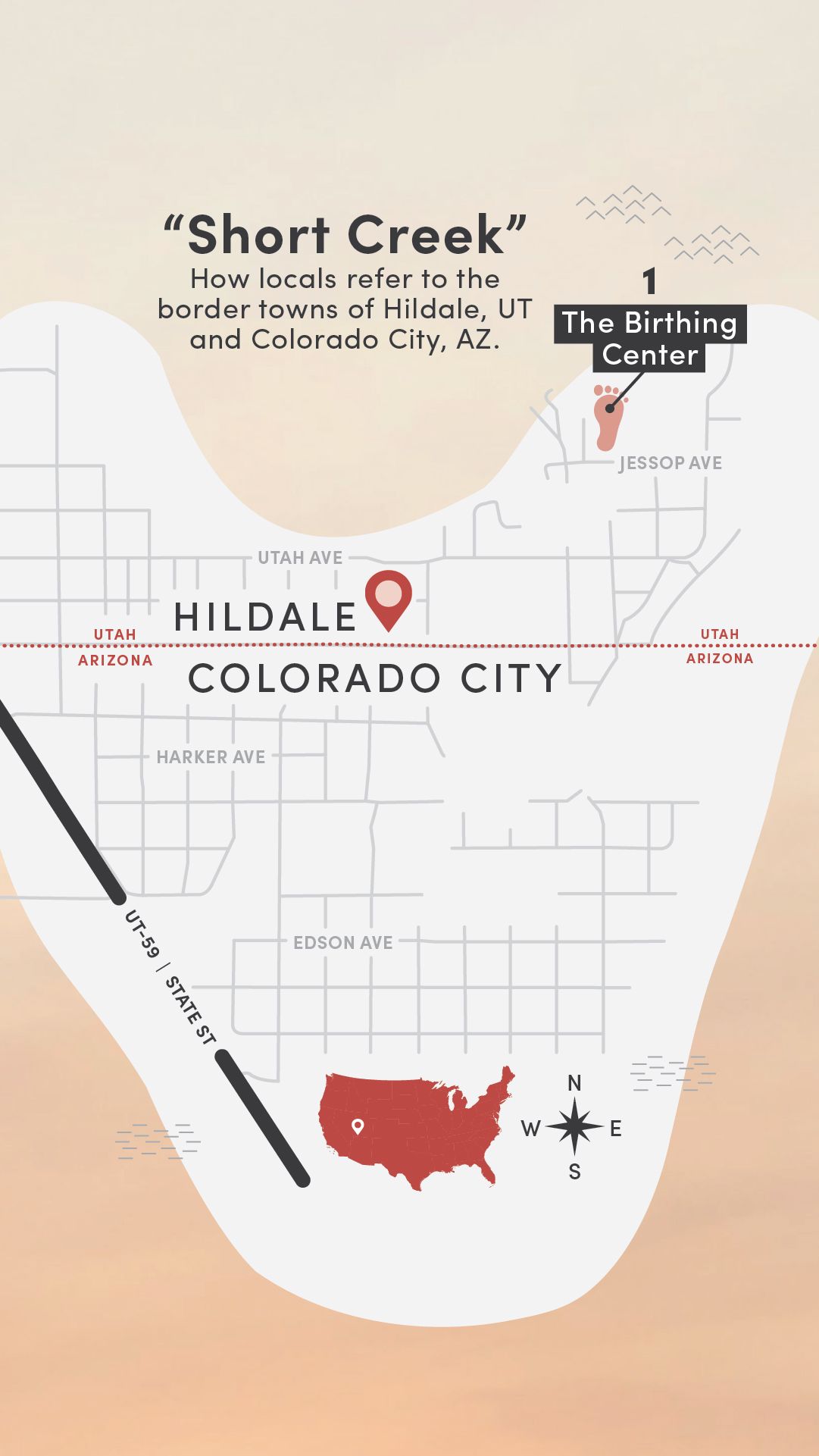
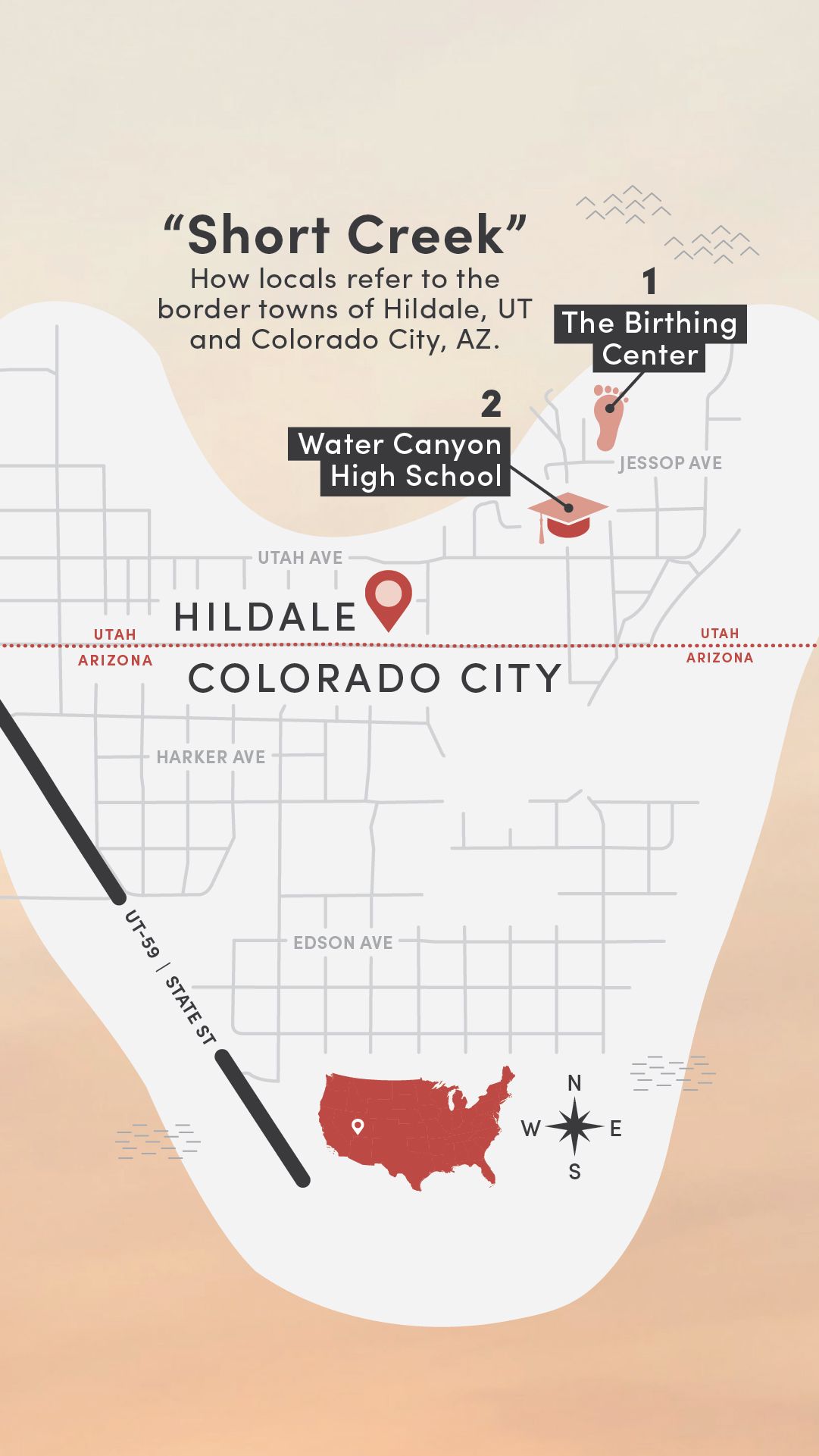

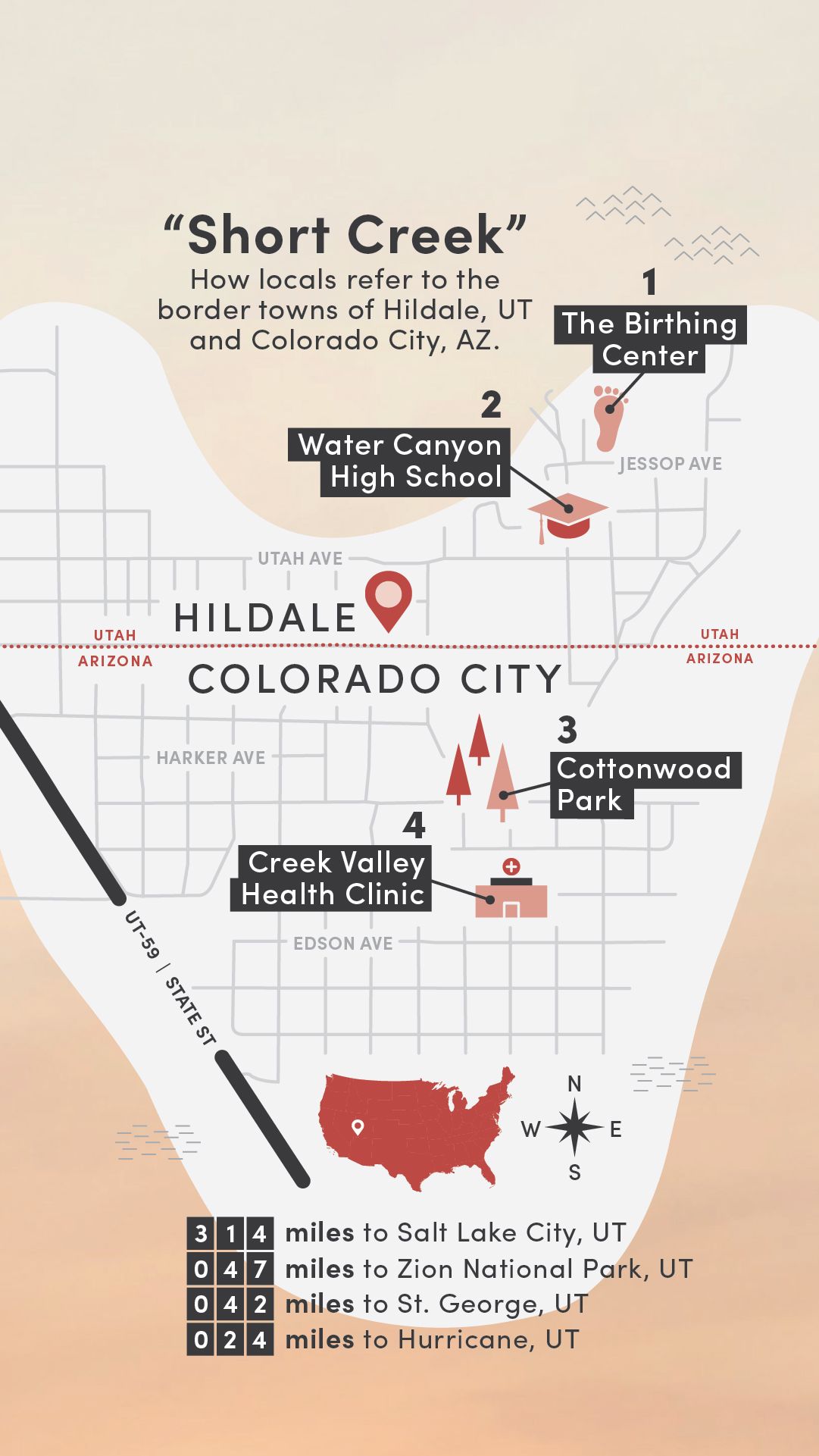
1. The Birthing Center
Historically, the main clinic in Hildale, Utah, was known locally as the birthing center. “Aunt Lydia” Jessop delivered thousands of babies there until her death in 1996. After Warren Jeffs became prophet in 2002, access to health care became increasingly restricted.
2. Water Canyon High School
The high school agreed to host the health fair in its gym, with the locker rooms available for physicals. Bennett, Draper, and Merrill invited service providers to man booths, and a group of first-year U of U Health PA students signed up to help just weeks into their courses.
3. Cottonwood Park
Long a place for celebration and gathering for communal parties and parades, Cottonwood Park fell into disuse in the 2000s. In 2018, the park was renovated with fresh sod and a playground and now stands as a flagship for municipal and community efforts to rebuild the Creek.
4. Creek Valley Health Clinic
Incorporated in December 2018, Creek Valley Health Clinic was the brainchild of Steed, Draper and Knudson, among others who championed the idea of opening a clinic with staff and a board drawn from the community who understood its unique needs and history.
Some community leaders had been working with a federally funded, St. George-based health care network to open a satellite clinic in Short Creek. Among them was local non-profit Cherish Families, which had been gathering data to underscore the community’s need for health care. But the effort to open a clinic was dogged by many questions.
Would a community health clinic be able to overcome the community’s deep, bitter divisions, let alone address the generations of trauma that afflicted so many?
Mental health has long been the biggest concern the community faces, and Utah’s Southwest Behavioral Health fought hard to help, bringing in independent contractors to work with women and men struggling with trauma from their former lives in the FLDS.
Steed points to the decades when families were separated by the church’s leadership under Warren Jeffs. Male teens and young men were driven out. Those in the FLDS ranks deemed as unworthy, nonconformist, or rebellious recall former members were isolated, shunned or exiled. Some fled, others stayed, only to face in some cases stricter demands on their loyalty and behavior.
Wounds from those times still linger. When Steed's family had moved to Centennial Park, his grandmother had remained with the FLDS. Steed used to meet her every couple of months in Cottonwood Park, bringing her flowers. After his first daughter was born, she gave him a blanket. “This is the last time we get to meet together,” she told him.
It’s not just the neglect, ostracization, and trauma that many cite, nor the poverty and isolation. “As a teenager, I would have loved to have someone to talk to,” Steed says.
“Really, we live quite unique lives. There were stressors that we dealt with that are hard for anyone else to relate to unless they had cultural experience and training about the area.”
Steed argues a health clinic is the only thing that could overcome all the deep fractures that run through the community.
“It’s the only institution that is available to everyone that provides such a benefit. If your kid needs stitches, you’re going to prioritize that over what religion the person giving the stitches is. At least I think you will.”

Come to the Fair

IN LATE 2017, RICHARD BENNETT FROM U OF U HEALTH REACHED OUT TO SHIRLEE DRAPER, DIRECTOR OF OPERATIONS OF CHERISH FAMILIES, AND NEWLY ELECTED HILDALE MAYOR DONIA JESSOP—THE FIRST WOMAN AND FIRST FORMER FLDS MEMBER TO EVER TAKE OFFICE IN THE TOWNSHIPS—TO ASK A SIMPLE QUESTION: “IS THERE ANY WAY WE CAN HELP THE COMMUNITY?”
He’d seen the two women present on cultural competency when interacting with former and current FLDS members, “who are so highly attuned to any kind of paternalistic attitude toward who they are,” Draper says. That's why providers need culturally competent training. “It means they are able to provide empathetic and non-judgmental support and help.”
Shirlee Draper at the offices of non-profit Cherish Families
Shirlee Draper at the offices of non-profit Cherish Families
In January 2018, Bennett met with Jessop and Draper in his St. George office. Why did he want to help, they asked? He talked about growing up in Hansen. They understood, they told him. They’d grown up in Short Creek, and its red dirt also drove them to want to give back to their hometown.
Bennett’s idea was to try a health fair—a standard tool for introducing services to an area that doesn’t have them—as a way of supporting the nascent clinic plans. “Our first health fair was to try to embrace that idea of bringing that clinic to the community,” Bennett says. “To see patients, show them what services were available, and funnel them into long-term relationships with network providers.”
Richard Bennett one summer afternoon in Cottonwood Park talking with the story's author.
Richard Bennett one summer afternoon in Cottonwood Park talking with the story's author.
When Bennett suggested a health fair, it was a light bulb moment for Draper. With the next school year soon to start, there was no way for Creek mothers to get their children physicals or screening for vision or hearing problems, as well as fluoride varnishing for their teeth (local concerns over radium in the water meant only bottled water was consumed). It would be an opportunity for locals to get basic health screenings for free in one location, she thought.
Water Canyon High School agreed to host the health fair in its gym in July 2018, with the locker rooms available for physicals. Bennett, Draper, and Merrill invited service providers to man booths, and a group of first-year U of U Health PA students signed up to help just weeks into their courses.
The 19 students attended Draper’s presentation on plural family cultural competency.
The evening before the fair, she also led a bus tour through the townships’ largely unpaved streets, past houses that, from the outside at least, appeared abandoned or unfinished, many half-hidden behind corrugated fences.
It felt like a surreal ghost town to the students, the streets empty of people, yet full of curious sights: dozens of washing machines lined up in front of one house, horses galloping along the street, a young woman on a swing, the dying sun glinting in her long, ornate braids.

THE DAY OF THE FAIR, U OF U HEALTH’S PA STUDENTS SET UP BOOTHS, ORGANIZED DONATION BOXES, AND TOOK PATIENTS’ VITAL SIGNS. STUDENTS WERE STRUCK BY HOW LOCALS, SOME IN PRAIRIE DRESSES AND ELABORATE HAIRDOS, THE BOYS IN FLANNEL SHIRTS AND JEANS, WALKED TENTATIVELY INTO THE GYM AS IF ONTO A STAGE.
They seemed distrustful, exposed, and vulnerable, some simply standing in a group for an hour or more, taking it all in. Others were less standoffish. Jordan Merrill invited a man in his late 50s to have a screening. “Sure, I never had that done before,” he said. “Let’s give it a try, see where we’re at.”
All the adults and children had a heartbreaking story they wanted someone to listen to, Bennett found. The locals wanted providers to understand what it meant to them that they were there and why they felt the way they did.
With 400 care visits for the 200-plus fair attendees, the fair’s success stunned its organizers. Now community leaders had raw data that underscored the demand for a clinic.
Tyler Steed called the health fair “a massive blessing. To offer health care that was non-discriminatory, including to people who cannot afford health care, opened people’s eyes and opened doors.”
By fall 2018, Knudson’s championing of a clinic with staff and board members drawn from the community who understood its unique needs and history had gained significant support. Community leaders rallied around this new approach.
Steed, Draper, and Knudson, among others, incorporated the Creek Valley Health Clinic (CVHC) in December 2018.
The next step was to apply for a federal Health Center Program New Access Point grant to fund a federally qualified health center (FQHC). Only five slots nationally were available to fund new FQHCs not already members of the program. CVHC was the only “paper-start” organization, meaning that it was not already in operation at the time the funding was to be awarded.
The grant had to be in the following April. Luckily, CVHC already had their first employee in mind. Hunter Adams grew up in Salt Lake City and attended Utah Valley University, where he met his future wife, a member of a former FLDS family. Adams worked in population health analytics and decision support for Intermountain Healthcare in Salt Lake City. He had taken part in early discussions about opening a clinic with Knudson and community leaders.
Hunter Adams showing visitors around the back rooms of the Creek Valley Health Clinic.
Hunter Adams showing visitors around the back rooms of the Creek Valley Health Clinic.
Adams took on the role of jump-starting what would have to be a robust clinic. In total, they would be required by the federal Health Resources & Services Administration to offer 19 services themselves or through a third party. The services focused on primary care, newborn visits, wellness checks, procedure-based medicine, vaccinations, behavioral health care, and preventive dental care, along with transportation for patients unable to come to the clinic and health education training classes.
Knudson credits two people with getting the clinic renovated and open: Hunter Adams and local resident JoAnne Zitting, the latter donating her time and community connections to getting the clinic open. Adams and Zitting were the primary writers of the grant, “and effectively were the clinic in the days before it was federally funded,” Knudson said. In just three months, they had the 158-page application submitted to the federal government, five days before the mid-April deadline.
Second Time Around

AS THE JULY 2019 DATE FOR THE SECOND HEALTH FAIR APPROACHED, SECOND-YEAR PA STUDENTS WHO HAD ATTENDED THE FIRST CLINIC SIGNED UP TO DO PHYSICAL EXAMS, AND SEVERAL U OF U HEALTH PROVIDERS AGREED TO TAKE PART.
Jennifer Leiser, MD, Clinical Professor of Family Medicine at University of Utah Health, would provide women’s health care for a community where many women had not had a gynecological exam in 15 years. Jeri Bullock, DDS, associate professor in the School of Dentistry, committed to dental care.
Much like Bennett and Merrill, Bullock’s passion for the underserved goes back to her childhood in a rural town. In her case, it was southern Nevada’s Moapa Valley, so small it didn’t even have a stop light. Her family lived in a single-wide trailer, and while her truck driver father earned enough to lift them above the federal poverty level, they barely scraped by.
Compared to the cautiousness many locals displayed at the first fair, “There was a tangible buzz in the room” at the second, Merrill says.
Volunteer dental students and U of U Health School of Dentistry staff outside the high school where the health fair took place. Left to right, Jeri Bullock, DDS; dental assistant Whitney Haydock; and students Cory Johnson, Taira Graves, Campbell Moore, and Maggie Rodriguez
Volunteer dental students and U of U Health School of Dentistry staff outside the high school where the health fair took place. Left to right, Jeri Bullock, DDS; dental assistant Whitney Haydock; and students Cory Johnson, Taira Graves, Campbell Moore, and Maggie Rodriguez
Bullock, along with a small team of four dental students and a dental assistant, saw patients in the high school’s home economics room. What they found was worse than Bullock had expected. “Many of the families have limited financial resources and are not on Medicaid, so only emergency dental treatment is utilized,” Bullock wrote in her report.
“This was the first dental experience for many of the children.” In total, 18 patients had signed up for dental care at the fair.
“With the overwhelming dental need, we nearly doubled the expected patients, with 32 people receiving treatment.”
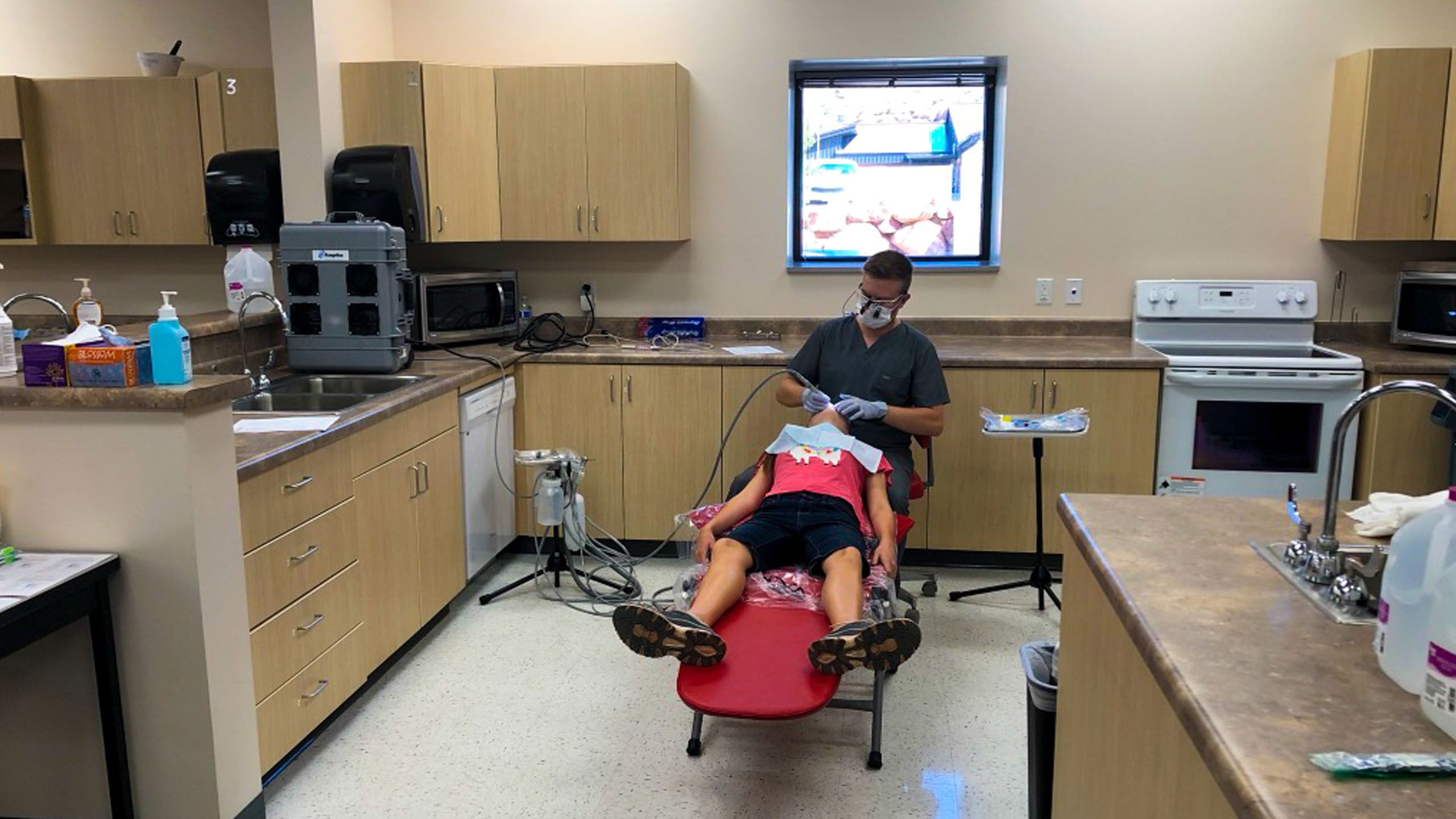
WHAT STRUCK BULLOCK WAS HOW LOCALS REACTED TO THE LONG WAIT TIME. TYPICALLY, AT HEALTH FAIRS, PEOPLE BECOME IMPATIENT AND ANGRY AT AN HOUR WAIT. BUT NOT IN HILDALE.
Families worked together to entertain the many children, allowing someone to move ahead if they had a prior obligation while watching over each other’s children as they received services. The sense of community reminded her of Moapa Valley. “They were so appreciative of us being there,” Bullock said. It was a breath of fresh air, honestly.”
In the first hours of the fair, out-of-town providers felt they were stepping on eggshells. But as they had conversations with locals, barriers went down on both sides.
“You felt even if it didn’t change your life by taking someone’s blood pressure, it changed their perspective by the interaction they had,” Merrill says.
For U of U Health PA students, the health fair’s impact went far beyond that. In follow-up reports, students expressed how the day-long event had “set the foundation and mindset that will last the rest of my career,” one wrote. It taught them cultural humility and compassion for those with a starkly different background.
At the fair, Bennett felt like a parent watching a child grow up and realizing they were a good person. It was a snapshot of who the students truly were, he thought, as one knelt next to a child, helping them cover one eye for a vision test.
“They aren't interested in the unique culture that these patients grew up in,” he says. “They just know this kid needs health care, this person needs someone to listen to them, and they do it.”
For Knudson, the second health fair was particularly useful for the emerging clinic because Bennett and University of Utah Health agreed that it should run under the Creek Valley Health Clinic brand.
“We were still just getting our feet underneath this,” Knudson says, “and University of Utah and Richard Bennett were very generous in basically taking on all the costs and allowing Creek Valley to take all the credit.”
From a community outreach perspective, having the yet-to-open clinic’s name on the fair helped to solidify its presence in Short Creek.
A Question of Faith

WHETHER ACTIVE FLDS MEMBERS ATTENDED EITHER FAIR WAS DOUBTFUL, ACCORDING TO COMMUNITY LEADERS. ATTENDANCE WOULD HAVE GONE AGAINST CHURCH MANDATES TO NOT MINGLE WITH OUTSIDERS OR APOSTATES.
In late 2019, a small group of FLDS women interviewed for this story explained why such doubts were warranted. They talked about how they, their children, and grandchildren had also experienced trauma, albeit from a different source than former members. Their trauma stemmed from being repeatedly evicted by a local land trust for non-payment of property taxes on their homes and losing buildings fundamental to their faith.
The latter concern in particular brought out heated emotion as the women criticized both the fairs and the proposed clinic. Their concerns focused not on the medical activities, but rather where they took place. Those locations were buildings the FLDS view as sacred.
The high school where the fairs took place had in a prior incarnation been the FLDS Bishop storehouse. The single-story building that was to house the proposed clinic was in Colorado City. The FLDS had called it “The Annex,” and it had provided urgent care during the hours the Hildale birthing center was closed. Another site of contention was the birthing center in Hildale, partly given over to administrative offices for the nascent clinic.
The women would never enter the buildings again, they said, until control of the properties returned to their church.
Faith wasn’t the only issue stopping them from accessing future services. They worried about how applying for health insurance might trigger an unwarranted investigation into their finances, child-rearing, or home-schooling.
Then there were concerns with the providers. They didn’t trust those who had connections with the community, so why would they trust their health care advice? “It’s run by people that are avowed apostates and enemies of anything to do with our religion,” Richter said. A primary mandate of their faith, which Richter attributes to Brigham Young, second president and prophet of the Church of Jesus Christ of Latter-day Saints, is to shun apostates “severely.”
Confronting the Past

IN SEPTEMBER 2019, HUNTER ADAMS LEARNED THAT CREEK VALLEY HEALTH CLINIC (CVHC) HAD BEEN AWARDED A $650,000 ANNUAL ACCESS POINT GRANT TO OPEN A NEW FQHC. THEY HAD JUST 120 DAYS TO DO IT.
The key from the beginning was that the clinic stood apart from the often-tortured, highly personalized politics of the small townships. While some who are involved are part of a plural family community, and others had left that culture, the clinic couldn’t be seen as affiliated with a particular church or organization.
“Having that independence was so important,” Tyler Steed says. “Otherwise, we would have immediately alienated a large percentage of our patient base, which would have undermined the clinic’s long-term sustainability.”
At the same time, the clinic needed providers who understood the unique history and needs of the community—who would answer the call of the red dirt in their veins. In CVHC physician assistant Nathan Barlow, they found one such provider.
Barlow left Short Creek when he was 24, swearing he’d never return. After a spell in the army, he went to PA school at the University of Washington and did his clinical training in Hawaii, four months of which were spent in a small, rural town with a clinic much like CVHC in both scale and mission.
Nevertheless, he was hesitant when CVHC asked if he was interested in returning to join them. As the oldest of 16 kids, his mother, sisters, and old friends were still FLDS and didn’t talk to him. But he saw it as an opportunity to mend fences and build bridges.
Barlow’s more than aware of the health challenges in his community—particularly mental health. “It's one of the biggest issues the majority of us have here,” he says. “So many people repressed difficult memories and try to act like everything is OK, and it’s not.”


For Barlow, it’s more than a job. He came back to be part of the healing and, in the process, found old friends and made new ones.
He also put his own demons to rest. “I believe many of my patients are finding that same healing as they open up.”
Just in Time

THE CREEK VALLEY HEALTH CLINIC OPENED ON DECEMBER 16, 2019, WITH A RIBBON-CUTTING CEREMONY AND, AT FIRST, A SLOW TRICKLE OF SCHOOL-AGE PATIENTS WITH CUTS, BRUISES, AND THE ODD BROKEN LIMB FROM DIRT BIKE AND HORSE RIDING ACCIDENTS.
Adams, now CEO of CVHC, stresses that the clinic is for everyone. “If you have a sick child and don’t know where to turn, we are here to serve you and your family. No matter where you are in life, no matter your background, your income or insurance status, we’re here for you.”



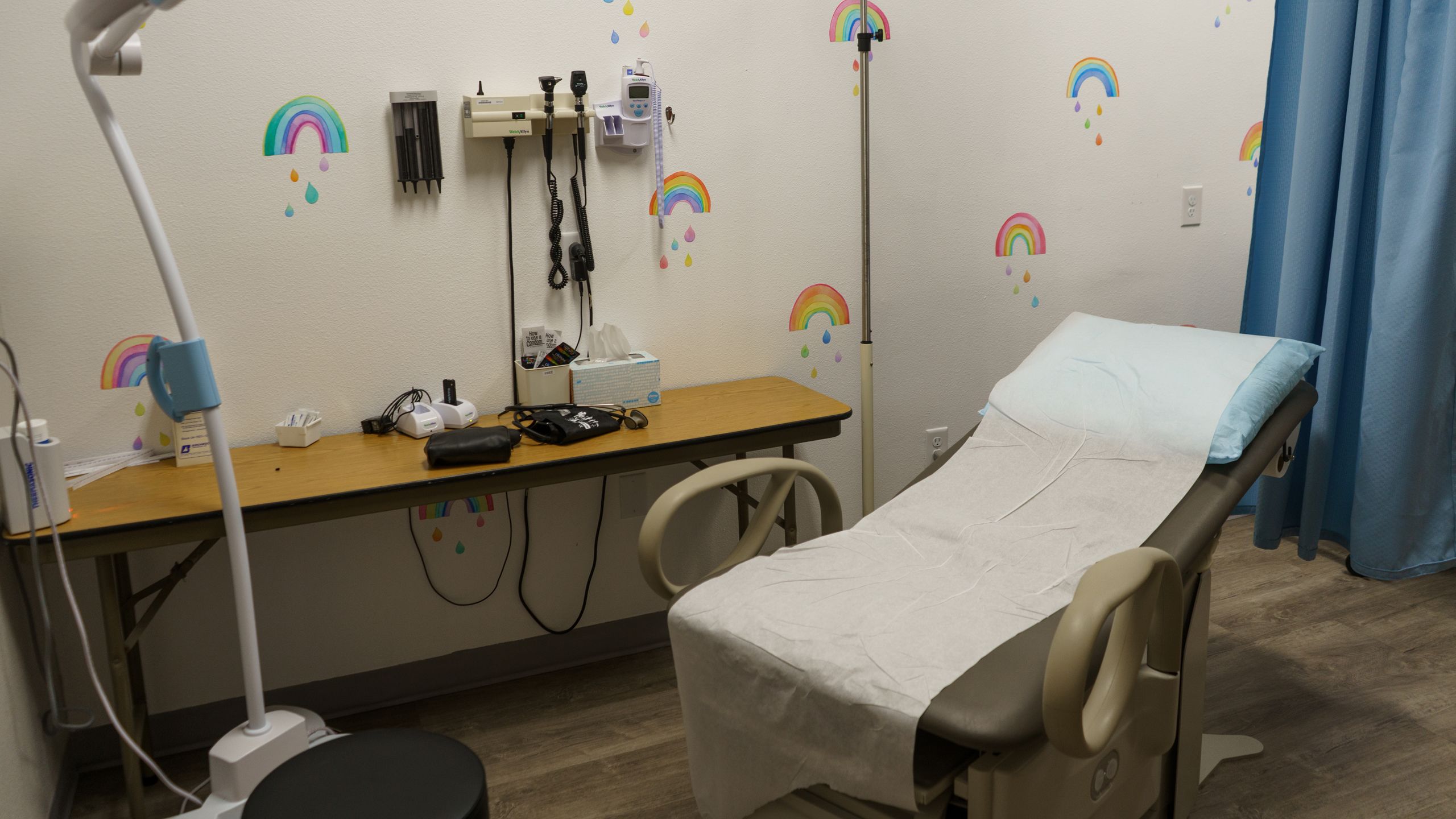
THE NUMBERS OF PATIENTS BEGAN TO GROW, BUT ONLY FIVE MONTHS AFTER OPENING, THE COVID-19 PANDEMIC HIT UTAH. THE LOCKDOWN STRESS SO MANY EXPERIENCED ACROSS THE BEEHIVE STATE WAS ONLY MAGNIFIED IN SHORT CREEK BECAUSE OF ITS ISOLATION, HISTORIC FEAR OF GOVERNMENTAL INTRUSION, AND OMNIPRESENT TRAUMA.
That isolation kept the virus at bay through the summer as the clinic continued to grow. By October 2020, CVHC had treated 2,000 patients and grown to 25 employees. Then, a month later, COVID-19 swept through the community, and the clinic found itself doing more tests than the rest of the year combined. They were one of the few clinics offering free tests in the St. George district. “Our small size allowed us to adapt to all the changes, providing testing and vaccines,” Adams says. “In that sense, we had the clinic here at the perfect time, when the community needed it most.”
U of U Health students from Bennett’s program rotated through the clinic in the second half of 2020. Along with patient care, they learned how to negotiate deeply rooted anti-vaccination sentiments among patients. They also had to learn about unfamiliar flora and oils that some locals relied on for their home health care.
Lissande Tokorcheck, then a PA student at U of U Health, had worked both health fairs and was struck by the lack of health knowledge and poor dental and physical care she had encountered. The first day she drove to the clinic to begin a two-month rotation, her feeling of being in a foreign land was only exacerbated by the deserted basketball court she passed. A huge tractor wheel dominated the court, next to garbage piled up underneath one of the hoops.
At the beginning, she was overwhelmed by the desire to be respectful and not tread on anyone’s toes in a culture she felt she barely understood. Over time, she appreciated the commitment so many in the community had to each other, a form of grave grace that spoke to decades of weathering the Short Creek’s challenges.
One woman came in multiple times with different girls, and Tokorcheck learned she took care of many children, not all of whom were her own. While the woman’s life was one of poverty and demanding responsibilities, Tokorcheck was moved by the sense of family that bound her to all the children—and them to her.
Caring for Teddy

IN AN ENCLAVE THAT PRIDES ITSELF ON SELF-DETERMINATION, IT'S NOT ONLY FORMER FLDS AND CENTENNIAL PARK MEMBERS WHO HAVE GONE THROUGH MEDICAL SCHOOL AND NOW CARE FOR THOSE THEY GREW UP WITH. THE FLDS ALSO HAVE PROVIDERS THEY RELY ON WHO COME FROM THEIR OWN RANKS.
Many FLDS women have gone into health care, studying at nursing school or university and then working as nurses, providers, or, in 24-year-old Louisa’s case, as a respiratory therapist.
Louisa’s mother, Norma Richter, studied speech therapy at the University of Utah (alum 1991) because there was a community need for such skills. Louisa’s inspiration was her younger brother, Teddy, one of 11 siblings. (Louisa requested anonymity for this story.)
Born hydrocephalic in 2000, Teddy was diagnosed with a congenital brain malformation, Dandy-Walker’s syndrome. When they weren’t taking Teddy to specialists at a Phoenix hospital, the family cared for him at home. Her mother taught 8-year-old Louisa how to turn his pump on and off and take care of his feeding tube. “I wanted to know,” Louisa says. “I wanted to do it.”
When Teddy was 18, he suffered an anoxic brain injury, depriving the brain of oxygen, shortly after the funeral of Richter’s oldest son, who had died in a motorbike accident.
After Teddy came home from the hospital, Louisa, then working as an EMT, CNA, and patient care tech in St. George, realized she could help her brother even more if she learned more about his needs. In May 2021, she graduated as a respiratory therapist.

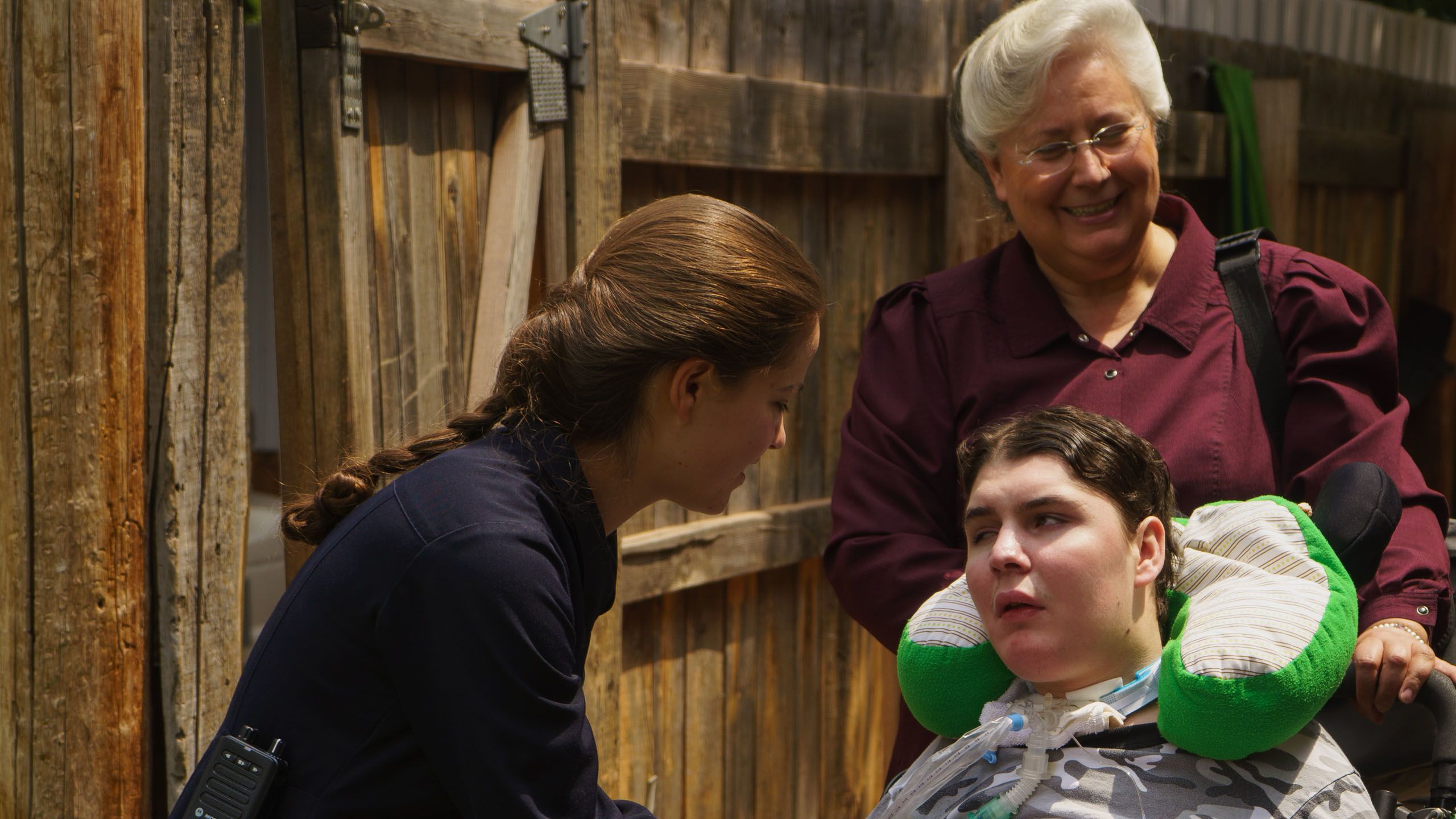
LIKE HER MOTHER, LOUISA WON’T GO TO CVHC FOR CARE FOR RELIGIOUS REASONS.
BUT SHE HAS NOTHING AGAINST THOSE WHO CHOOSE TO GO THERE. “I THINK IT’S A GOOD RESOURCE FOR THEM.”
AS MUCH AS LOUISA RESPECTS OTHER PEOPLE’S BELIEFS, SHE NEVERTHELESS KEEPS HER FAITH TO HERSELF AT WORK. “I WORK IN EVERY SINGLE UNIT IN THE HOSPITAL. A LOT OF FOLKS DON’T KNOW WHO I AM.”
She and other family members have had to put up with discriminatory comments and attitudes about the FLDS. It’s also a question of safety, she says, especially after a Cedar City man was jailed in early 2020 for threatening to kill “polygamists.”
When Louisa walks into the hospital in scrubs, she’s one more health care professional. But “if I show up in a dress,” she says, “people treat me like I’m dumb, like I’m uneducated and don’t know what I’m talking about.”
That stark contrast became all too apparent to her when she went to the hospital with a family member, both in FLDS garb, to give someone a gift, only for everyone they passed to stare at them. “I walked down that same hall yesterday in scrubs and nobody stared at me at all.”
Shoeless in Colorado City

ON JUNE 9, 2021, RICHARD BENNETT DROVE FROM HIS ST. GEORGE HOME TO CREEK VALLEY HEALTH CLINIC TO BEGIN HIS FIRST DAY VOLUNTEERING AS A PHYSICIAN ASSISTANT. AS HE THREADED HIS WAY THROUGH THE MOUNTAINOUS LANDSCAPE, HE THOUGHT BACK TO WHEN HE FIRST SHADOWED A PA IN CHOTEAU, MONTANA. THAT WAS WHEN HE REALIZED THIS WAS HIS TRUE ROLE IN LIFE—CARING FOR HIS PEOPLE, THE RURAL POOR.
The prospect of his first day at the clinic had made him nervous, but he had nevertheless bought new shoes to mark the occasion.
Bennett turned off Central Avenue and swung into the clinic’s car park. He looked to the north, to the majestic red cliffs that protected Short Creek from the outside world. He never wanted to take for granted the timelessness of this place.
A mother brought in her bright, chatty 9-year-old son for a check-up. The boy sat on the examining chair and Bennett glanced down at his swinging feet.
His shoes had barely any sole left, his dirt-red toes sticking out the front. Bennett looked at his own brand-new shoes, then at his patient’s remnants, and thought, “I’ve got to do more, it’s not enough.”
As those first months attending the clinic wound on, Bennett became enamored with the staff’s passion for the community—and with the community itself.
By the end of the year, he’d realized that, as much as he wanted to do more for Short Creek, he was missing the point. The clinic had always been the missing link for the community, but it also completed in a personal sense the circle to the question he’d asked at the beginning: “How can we help?”
In mid-January, he decided to leave U of U Health’s PA program, which had so inspired him to do more, and dedicate himself full time to Creek Valley Health Clinic.
Each day, Monday through Friday, he goes into a patient room, stethoscope around his neck, and answers the call of the dirt in his veins.

Story by Stephen Dark
Design by Jessica Cagle
Images of Short Creek by Tolgas Katas and Stephen Dark.
Images of the Bennett family provided by Richard Bennett.
Photos of Dentistry staff and students courtesy of University of Utah Health School of Dentistry.
Stephen Dark would like to thank Christine Marie Katas of Voices for Dignity for her help with part of this story.







