First Steps to Redemption (COPY)




By Elaine Jarvik
March 27, 2026
To reach Decker Lake Youth Center, drive past the lake itself, where on a sunny afternoon you might see picnickers and joggers enjoying the park. Next door, the Youth Center sits behind tall, barbed-wire fences, with no view of the park or water at all.
Enter the main building, walk through a metal detector, put your phone in a locker, wait to be escorted through three locked doors, and you'll come to the office of Sandy Rutledge, ADN, RN, CCHP. The incarcerated youth call her “Nurse Sandy,” with obvious affection. They give her fist bumps whenever they see her.
Sandy Rutledge, ADN, RN, CCHP, inside the community room at Decker Lake Youth Center.
Sandy Rutledge, ADN, RN, CCHP, inside the community room at Decker Lake Youth Center.
“I never look up what they’re in here for, because I don’t want to have any bias for the nursing care they receive.”
Rutledge has worked in the all-male Decker Lake Youth Center for three years and is one of nearly 50 health care professionals who comprise the collaboration between the University of Utah College of Nursing and Utah’s Division of Juvenile Justice & Youth Services (JJYS). Like other nurses and physicians who treat incarcerated youth, she has one rule for herself: “I never look up what they’re in here for, because I don’t want to have any bias for the nursing care they receive.” The patients she treats, she says, “should receive the same care as someone who’s not incarcerated, with no judgment.”
Indeed, ever since the 1976 Supreme Court ruling in Estelle v. Gamble, states are required to provide “adequate medical care” to all incarcerated individuals as an Eighth Amendment right. Rutledge adds “no judgment”—especially for a population so often stereotyped, overlooked, and stigmatized. “I always think, ‘What if these were my boys?’” says Rutledge, who has five grown children of her own. “‘How would I want them to be treated?’”
Decker Lake is one of fivesecure facilities and seven detention centers operated by JJYS across Utah. As a group, these facilities are called “Youth Centers,” the terminology used on signs posted at every entrance. The system is run by the Utah Department of Health & Human Services (DHHS), not the Department of Corrections, shifting the focus to rehabilitation rather than punishment—a trend reflected by national and state-level statistics.
That allows staff to deliver enrichment, education, and self-determination to incarcerated youth. Nurses care for the physical and mental health of the youth while coordinating dental services, nutrition classes, and health literacy education.
It’s one of the longest-running community engagement partnerships at the University of Utah. The College of Nursing has maintained its contract with DHHS for over 26 years. The arrangement is unique: the college staffs registered nurses (RNs), family practice nurse practitioners (FPNPs), psychiatric mental health nurse practitioners (PMHNPs), and medical assistants (MAs) within the walls of the facilities. Although clinic hours vary, RNs, FNPs, and PMHNPs are typically present during working hours. There’s no 24-hour infirmary, but on-call services are provided after-hours to assess and treat health problems that may arise or manage new admissions, which may take place overnight.
“Nurses view people holistically,” says Marla De Jong, PhD, RN, CCNS, FAAN, dean of the college. “We want the best possible health outcomes for all people—that’s why nursing is one of the most trusted professions. These youth in the juvenile justice system are, first and foremost, young people. They are more than their circumstances—each with a story, ambitions, and goals—and they deserve to be treated with dignity and compassion. Their health and wellness are just as important to us as the health and wellness of any person.”
“These youth are more than their circumstances—each with a story, ambitions, and goals—and they deserve to be treated with dignity and compassion.”
The partnership benefits everyone—including the next generation of nurses. College of Nursing faculty work on-site, providing instruction to registered nurse (RN) and nurse practitioner (NP) students. All 12 JJYS facilities serve as clinical placement sites where preceptors instruct these students on how to work with a unique population outside the hospital setting.
Under the direct supervision and guidance of licensed RNs and NPs, students explore health issues that impact adolescents. They learn to communicate across a range of topics while maintaining a trauma-informed approach to care. They learn how to build trust with teenagers—never easy in the best of circumstances, and particularly difficult as an authority figure in a detention facility—and encourage them to open up.
It’s the kind of work that contributes to national standards of care for adolescents, solidifies the University of Utah’s mission to serve everyone in the state, and aligns with nurses’ commitment to their profession.
One morning in early fall, Sandy Rutledge treated an adolescent who had suffered a knee injury playing basketball in the gym. She wanted to make sure he was doing OK, but what he really wanted to talk about was the hangnail that was bothering him. It’ll heal, she assured him, but she reminded him to keep his hands clean and, when cutting his nails, to make sure he cut them straight across. “And try not to bite them,” she added, while remaining focused on his injured knee.
The physical ailments that nurses address inside the juvenile corrections system include the common problems of any teenager—head colds, sprained ankles, stomach aches, and acne—along with more complex medical issues like diabetes, asthma, and congenital conditions like cardiac or gastrointestinal anomalies. Emergencies such as anaphylaxis or stage three hypoglycemia also occur, but are rare.
Being on site and available to the youth allows the nurses to build rapport. “What others may see as a suboptimal environment, nurses recognize as an opportunity to build trust and meet the health needs of detained youth,” Dean De Jong says. “Nurses have an opportunity to improve youth health, sometimes addressing long-standing unmet basic health needs resulting from limited access to health care.”
Inside the gym at Decker Lake Youth Center.
Inside the gym at Decker Lake Youth Center.
More often than not, incarcerated youth have a lifetime of trauma. They've seen people get shot. They’ve been shot at themselves. Maybe they were the ones who pulled the trigger. They’ve had friends or family members die in their arms. They may have endured failed adoptions and lived in multiple group homes. Many of the females have survived sexual abuse; many males have been in gangs. The daily presence of nursing staff provides reassurance, consistency, and stability.
When they’re first arrested and brought into a juvenile detention center, youth often arrive under the influence of marijuana, alcohol, or any of a multitude of legal and illegal medications. Sometimes they have injuries sustained during their arrest. Sometimes they are suffering the effects of homelessness.
If they arrive during the day, they are seen by a nurse within hours of admission. And if a detained youth arrives after hours, when medical professionals are gone for the day, the on-call nurse practitioner addresses critical medical and mental health issues.
Looking through a metal detector into the visitors’ waiting room at Salt Lake Valley Youth Center, a detention facility in South Salt Lake.
Looking through a metal detector into the visitors’ waiting room at Salt Lake Valley Youth Center, a detention facility in South Salt Lake.
“It seems like the youth overall have more mental and behavioral health needs than they did 10 years ago,” says Breck Bartholomew, RN, CCHP, nurse manager of the 12 youth centers operated jointly by the College of Nursing and JJYS. To meet those needs, the college and JJYS have added more mental health providers like Ally Cirenza, DNP, PMHNP, a board-certified psychiatric mental health nurse practitioner.
“There’s a lot of trauma walking these hallways,” says Cirenza, a 2024 graduate from the U’s College of Nursing who now works at Farmington Bay Youth Center once a week and fills in at Decker Lake when needed.
Like other psychiatric nurse practitioners caring for youth in these juvenile corrections clinics, Cirenza says she sees a common trifecta of mental health maladies: anxiety, depression, and post-traumatic stress disorder (PTSD). In addition, some youth live with cluster-B personality disorders—antisocial personality disorder, borderline personality disorder, narcissistic personality disorder. Self-harm behavior is also a prevalent concern for clinicians. In one instance, a youth even swallowed batteries and magnets and had to be taken to the hospital to have them surgically removed.
“We know from many years of research that the brain doesn’t continue to develop if it has experienced significant trauma.”
Michele de Leon Jauregui, MD

The young people in Utah’s juvenile justice facilities “are more likely to suffer from mental health conditions than the general population,” notes Michele de Leon Jauregui, MD, who has medical degrees in both pediatrics and psychiatry. Dr. de Leon Jauregui and Kristi Kleinschmit, MD, vice chair of education for Huntsman Mental Health Institute at the University of Utah and the Department of Psychiatry, provide consultation services for incarcerated youth with complicated health or mental health conditions.
“We know from many years of science and research that our frontal lobe doesn’t develop till we’re 25,” de Leon Jauregui says. “But it’s not just that. We also know from many years of research that the brain doesn’t continue to develop if it has experienced significant trauma. So just because you’re 17 doesn’t mean you’re developmentally 17, especially if you haven’t had adequate resources and haven’t been able to process what you’ve been through.”
Sometimes the stress of being incarcerated, plus anxieties about their crime, their future, and their family back home, leads incarcerated youth to experience high levels of cortisol, high blood pressure, sleeplessness, and nightmares. It can be stressful trying to sleep in a room that’s never completely dark so that staff can perform routine checks all night long.
Kalesita Nasilai, a unit supervisor at Decker Lake Youth Center, opens the door of a cell.
Kalesita Nasilai, a unit supervisor at Decker Lake Youth Center, opens the door of a cell.
A look inside a cell at Decker Lake Youth Center.
A look inside a cell at Decker Lake Youth Center.
Basic facilities inside a cell at Decker Lake Youth Center.
Basic facilities inside a cell at Decker Lake Youth Center.
“I really try to make them understand that the reason for their success is all the work they’re doing.”
Addressing these issues with the youth is the focus of the PMHNP and the JJYS therapy team.“I really try to make them understand that the reason for their success is all the work they’re doing” while incarcerated, says Valois Feneziani, DNP, PMHNP-BC, CCHP, a psychiatric nurse practitioner at U of U Health. “We get a handful of kids who think their success is tied to the medications they’ve been prescribed, and I really work hard to reframe that.”
In other words, empowerment—physical, mental, and emotional—is critical. Trauma-informed rehabilitation works hand in hand with accountability. Nurses encourage adolescents to exercise regularly. Gym class is a daily part of the school day, and offered on weekends and holidays. Youth take either high school or college classes five days a week, even in summer, along with life skills training and vocational instruction. And social workers hired by JJYS help with talk therapy once a week.
When he first arrived at the Salt Lake Valley Youth Center four years ago, John* says, “I started to spiral” and “I was on suicide watch for six months.” Now 21 years old, he credits therapy, “intense exercise,” meditation, and yoga for helping him survive. “You know you’re safe,” he adds, “and you know the staff cares.” He appreciates that Shannon Osburn, RN, a nurse at the center, sometimes even plays soccer with the teenagers.
These days, John serves on the detention center’s Youth Council, along with an 18-year-old. Today, they're laughing and expressing gratitude toward Shannon, who got the 18-year-old a wedge pillow to help reduce his loud snoring—something everyone on the unit appreciates.
Inside the nurses’ office at Salt Lake Valley Youth Center.
Inside the nurses’ office at Salt Lake Valley Youth Center.
Shannon Osburn, RN, sits at her desk in the nurses’ office at Salt Lake Valley Youth Center.
Shannon Osburn, RN, sits at her desk in the nurses’ office at Salt Lake Valley Youth Center.
These youth can find humor in tough situations. But there’s no denying the fact that some have committed serious crimes. That can make it hard for them to keep their cool—especially in the heat of the moment. One of the most frequent reasons for needing to see a nurse at Salt Lake Valley Youth Center, says Daniel Wixom, ADN, RN, CCHP, is a medical evaluation to assess for hand and wrist fractures from punching the cinder block walls.
Daniel Wixom, ADN, RN, CCHP, inside the nurses’ office at Salt Lake Valley Youth Center.
Daniel Wixom, ADN, RN, CCHP, inside the nurses’ office at Salt Lake Valley Youth Center.
Further education can help, as well. Following an initiative by the College of Nursing’s Quality Improvement Team, currently led by Feneziani, nurses have learned more about mindfulness meditation, “distress tolerance,” and emotion regulation. Many staff members are even trained in Dialectical Behavioral Therapy (DBT).
Let’s say some guy is annoying you, explains a 19-year-old who has been at Decker Lake for several years and has completed hours of DBT work. You could choose to fight the annoying guy, he says, or you could stop and think of the pros and cons of that choice. “When I was ‘out,’ I didn’t get that,” he says. “I would have liked to have learned that, how to keep my emotions down.”
JJYS takes further precautions to prevent injury. For example, couches are made of foam, without springs, because a spring could become a weapon. Nurses use multiple short wound wraps rather than an Ace bandage to wrap a sprained ankle, because youth could use Ace bandages to self-harm. There are no pencils, because youth can use sharp pencils to hurt others or themselves.
Inside the community room at Decker Lake Youth Center.
Inside the community room at Decker Lake Youth Center.
“Can you guys just fix my whole body? ’Cause I’ll never get medical care when I get out of here.”
Members of rival gangs are housed in separate units, and if a youth needs to get off-campus medical attention—a root canal, say—the exact day and time will be kept a secret, to make sure no gang members meet them at the oral surgeon’s office. If a youth needs treatment at any hospital or clinic, during transport, their feet and arms will be shackled, although every effort is made to cover these shackles in the hospital to decrease fear and judgment among others.
“People always ask, ‘Do you get scared working with these kids?’” says Radhika Makadia, DMD, who always answers, “No, they’re actually more afraid of me.” Makadia is a dentist hired to treat incarcerated youth in acollaboration with the University of Utah School of Dentistry, the College of Nursing, and JJYS.
Many incarcerated young people have never been to a dentist and have extensive untreated dental issues. For example, one youth arrived with 20 cavities and needed 13 teeth extracted. And even though they might have gotten multiple tattoos, some of them are afraid of needles. So Makadia starts by putting them at ease.
Recently, a 19-year-old came into Makadia’s office—just down the hallway from a mural that reads “There Is Beauty in the Struggle/You Just Have to See It”—for his biannual teeth cleaning. She remembered that he was taking a welding class, and when he sat down in her dental chair, she asked him about it.
Soon, as she and dental assistant Kate Kapinos poked, cleaned, and rinsed, the young man was happily chatting about how weird and cool it was that a big company like Yamaha makes both motorcycles and grand pianos. “I’m a nerd like that,” he said about his interests. Then the talk turned to airplanes, and he admitted that he’s afraid of flying. “Same with needles,” he said, then added, “But I’m getting past that.”

By and large, these adolescents enter the juvenile justice system having had little or no previous consistent medical care. Pre-arrest, if they were sick or injured, they usually either ignored it or went to the ER or urgent care. Sometimes, especially if they’ve lived in multiple group homes, they’ve been prescribed multiple psychotropic medications but don’t know why.
The bittersweet advantage of being incarcerated is that now these teenagers are never more than a day away from seeing a nurse and no more than a week away from seeing a primary care or psychiatric nurse practitioner. At the time of admission, nurses assess them for injury, illness, sexually transmitted diseases, and potential abuse. Family nurse practitioners may perform physical exams and provide primary or preventive care. Consistent with legal requirements, nurses and nurse practitioners, like other health care professionals, aremandatory reporters who must report suspected abuse or neglect when they encounter it.
Bartholomew remembers one youth saying, “Can you guys just fix my whole body? ’Cause I’ll never get medical care when I get out of here.”
There are limits, of course. Many youth ask for braces on their teeth, but, in most cases, braces are considered cosmetic—not the “ordinary care” guaranteed by law. The same goes for requests about teeth whitening.
Elizabeth Shvora, a student at the University of Utah College of Nursing, works at the Salt Lake Valley Youth Center.
Elizabeth Shvora, a student at the University of Utah College of Nursing, works at the Salt Lake Valley Youth Center.
Because these teens often don’t understand their own bodies, nurses try not only to treat but also to educate. For the most part, their health literacy is low, says Shannon Osburn, who works at Salt Lake Valley Youth Center while also pursuing a doctor of nursing practice degree at the U’s College of Nursing.
Makaeli Hopkin, RN, CCHP, who works at Slate Canyon Youth Center in Provo, recently began giving nutrition presentations at the state’s detention and secure facilities, bringing along the latest facts about healthy eating habits.
On a recent morning at the Salt Lake Valley Youth Center, Hopkin acknowledged that kids don’t get to choose what’s for dinner when they’re incarcerated—but they can choose how much they eat, as well as their snacks. Still, meals inside the facilities are healthy; breakfast and lunch must meet national dietary standards for school meals, while JJYS dietitians help to develop dinner menus.
Hopkin recommends “intuitive eating” strategies: paying attention to when they feel full and how different foods affect their health and mood. Her PowerPoint includes details about proteins, carbs, and healthy fats, along with the appropriate amounts of each that a teenager needs. The hope is that when they’ve served their time and return home, they’ll know how to make healthier choices for themselves and their families.
A classroom hallway inside the Salt Lake Valley Youth Center.
A classroom hallway inside the Salt Lake Valley Youth Center.
After a recent presentation, a youth approached Hopkin wanting to know whether it’s healthy if, “every day for five years straight,” a person drank Monster Energy drinks. “Hypothetically,” he added. Hopkin cautioned him that long-term consumption of high-octane energy drinks can cause heart problems.
In Utah’s juvenile justice system, wellness doesn’t end with physical and mental health or behavioral therapy. Nurses, teachers, and other staff know how important it is to empower the youth with vocational training, entertainment, and opportunities to still feel like a normal kid.
There’s a basketball court, a welding shop, and, in summer, a Slip ‘N Slide at Decker Lake Youth Center. Although incarcerated youth can earn the privilege of wearing headphones to listen to music, cell phones are not allowed—not just during school hours but 24/7.
Inside the gym at Decker Lake Youth Center.
Inside the gym at Decker Lake Youth Center.
Sandy Rutledge, RN, left, and Tom Rowley, NP, right, at the Decker Lake Youth Center in West Valley
Sandy Rutledge, RN, left, and Tom Rowley, NP, right, at the Decker Lake Youth Center in West Valley
The courtyard at Decker Lake Youth Center.
The courtyard at Decker Lake Youth Center.
Secure facilities like Decker Lake, in fact, represent both prison and possibility—in the same way that working as a nurse in a juvenile correctional setting is just like treating any other adolescent but also comes with its own peculiarities.
As Russell Murdock, who has worked as a medical secretary at the Salt Lake Valley Youth Center for 10 years, puts it: You have to have an unreliable narrator detector.
Russell Murdock, medical secretary at the Salt Lake Valley Youth Center clinic.
Russell Murdock, medical secretary at the Salt Lake Valley Youth Center clinic.
Breck Bartholomew echoes that: “The way many youth have been functioning in society or the world, I guess the best word is ‘manipulative’. We have to be very careful in how we assess and approach them, so we’re not being fooled too easily.” To get special treatment or medication—or a chance to travel to a medical facility on the outside—“they pick up on what you’re looking for and make it look like a problem when there’s not,” Bartholomew says. “Many youth can be like this, but others not at all.”
The youth do have the right to refuse treatment. “In corrections, there are very few things they have total control over, but health care is one,” Bartholomew says. Teens must assent to all care, and parents/guardians must give consent to any care beyond the “ordinary care” the state is mandated to provide. Consent must be obtained for vaccinations, prescription medications, and dental care. But the nurses try to explain to the teens why getting care is a good choice.
“I’ve had kids say, ‘I got mad at the staff this morning and that’s why I didn’t take my morning meds,’” Bartholomew says. “And I say, ‘Well, that really doesn’t benefit you, and it doesn’t punish the staff either.’”
What does benefit the incarcerated youth, however, is the College of Nursing’s academic expertise and dedication to current evidence-based care. Embedded in the correctional environment, CON faculty contribute to the growing field of correctional health care by participating in national conferences and boards. They hold seats “at the table” editing national standards for correctional health care. They can then bring this knowledge back to their students, both as preceptors and classroom instructors.
Given the circumstances and restrictions inherent in incarceration, correctional care is increasingly recognized as a specialty. Prior to holding their current job, none of the nurses at JJYS facilities were trained in this specific area. Once they begin working for the College of Nursing, they can obtain specialized training and certification through the National Commission for Correctional Health Care (NCCHC).
Jennifer Clifton, DNP, FNP-BC, CCHP-CP, CCHP-A, associate dean for practice and community collaboration in the College of Nursing, serves as the liaison between the American Association of Nurse Practitioners and NCCHC on the NCCHC Board of Representatives, serves as Vice Chair of NCCHC’s Juvenile Health Committee, and participated in the task force that revised the most recent juvenile corrections standards.
Nurses and other health care professionals lead initiatives on identifying and treating concussions, insomnia, and PTSD in incarcerated adolescents. Many have also received training in DBT and a technique called motivational interviewing.
The philosophy behind motivational interviewing is that “people inherently know what’s best for themselves,” explains Tom Rowley, DNP, FNP-C, CCHP, clinical director of the 12 JJYS facilities staffed by the College of Nursing. The idea is that collaborative, goal-oriented communication helps the youth pay particular attention to how they can change their behavior.
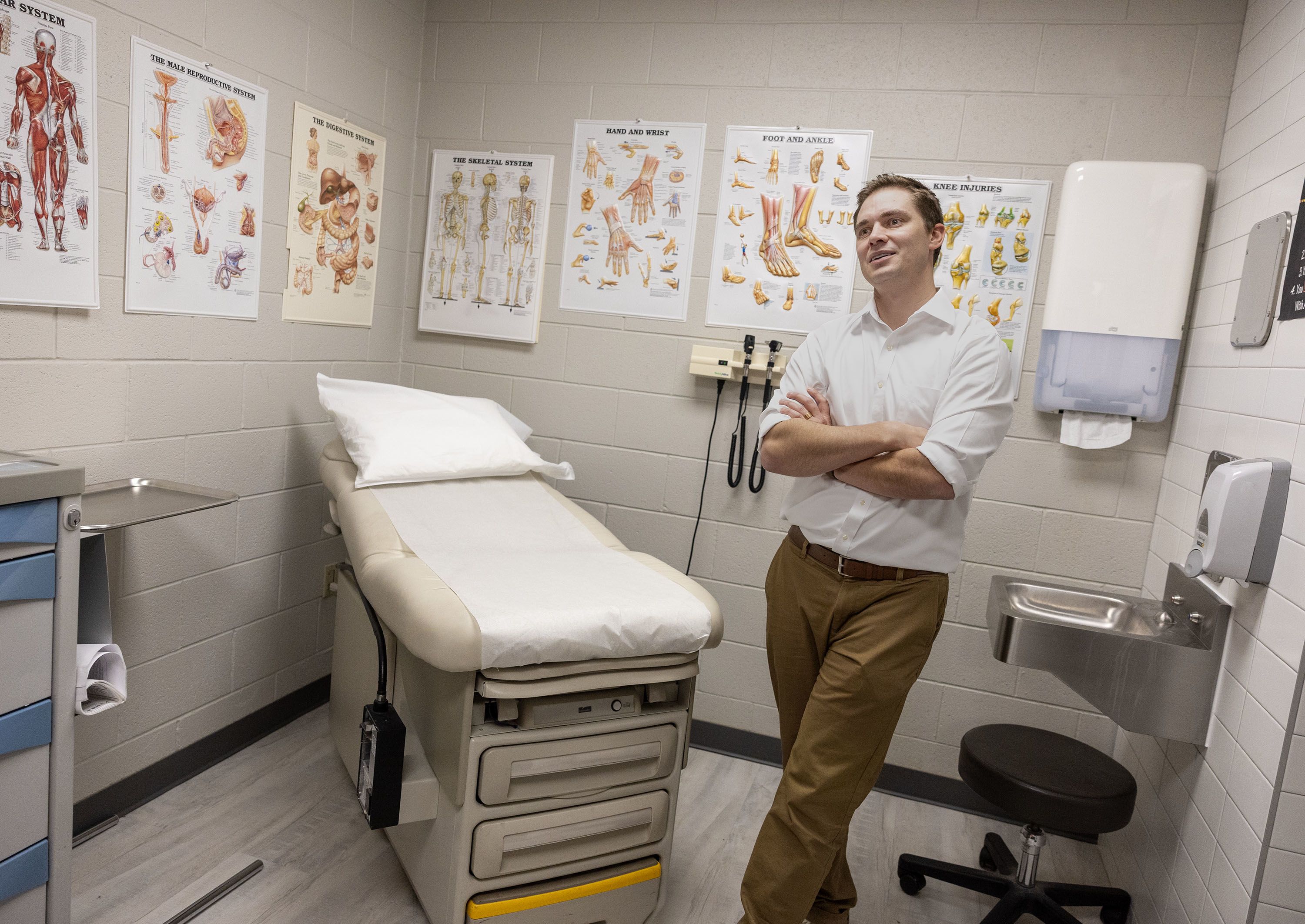
Tom Rowley, DNP, FNP-C, CCHP, in an exam room at Decker Lake Youth Center.
Tom Rowley, DNP, FNP-C, CCHP, in an exam room at Decker Lake Youth Center.
Instead of a lecture about the dangers of meth, for example, Rowley might ask why a drug is being used. Maybe the answer is “I want to forget about a death I saw.” When Rowley asks about downsides to using the drug, typical answers include “I can’t sleep very well and I’m not eating.” The goal is to help the youth find their own reasons to change.
Rowley, Feneziani, and Hopkin recently presented their studies on adolescent nutrition and DBT at the National Conference on Correctional Health Care; Clifton has also presented multiple times on the College of Nursing/JJYS model of care. This faculty participation elevates the CON, the University of Utah as a whole, and the state’s Juvenile Justice & Youth Services system, increasing national visibility, influencing correctional health standards, and advancing health care for Utah’s justice-involved youth.
“Our nurses practice with a high degree of independence and autonomy, delivering care at the full scope of their license,” Dean Marla De Jong says. “Across all JJYS facilities, they are the primary clinical leaders on-site. They are empowered to exercise sound clinical judgment and critical‑thinking expertise to meet complex health needs and position each youth for a successful and productive return to the community.”
On an early autumn day, Sandy Rutledge takes a seat at the edge of the gym inside Decker Lake Youth Center, behind rows of folding chairs set up for graduation. As she waits for the ceremony to begin, several youths spotted her and came over for a fist bump. Because some receive long sentences at Decker Lake, and because the state has raised the age an incarcerated youth can still be in juvenile custody from 21 to 25, Rutledge has known some of these youths for years.
Sandy Rutledge, ADN, RN, in the courtyard of Decker Lake Youth Center.
Sandy Rutledge, ADN, RN, in the courtyard of Decker Lake Youth Center.
The gym’s walls are covered in murals chosen and painted by the youth themselves. “Stay Motivated,” says one. “Family Connections,” says another, accompanied by a painting of hands curved in the shape of a heart.
When the graduation ceremony begins, a tiny recording of “Pomp and Circumstance” announces the arrival of two young men in caps and gowns, who walk across the gym floor and take seats next to the podium. They had recently completed coursework for a General Education certificate from Utah Tech University, and on this graduation morning, they received diplomas from Nathan Caplin, the co-founder of the Higher Education for Incarcerated Youth Program.
The mic didn’t work, but the two young graduates speak anyways. “I’ve never liked school,” one of them admits. “But I’ve been given a great opportunity, and I plan to use it. See you all for my associate’s degree!”
Drawings done by incarcerated youth decorate the hallways inside Salt Lake Valley Youth Center.
Drawings done by incarcerated youth decorate the hallways inside Salt Lake Valley Youth Center.
“It’s life-changing to see people who saw no future for themselves express long-term career and other life goals. The pride in the parents’ and guardians’ eyes is something I will never forget.”
These ceremonies are a big deal at Decker Lake, including high school graduations each spring. “Their parents, guardians, case workers, and staff members all attend, and most of us are in tears,” says Danielle Bennett, DNP, APRN, PMHNP-BC, a former psychiatric nurse student whose experiences working with incarcerated youth left a lasting impression on her. “It’s life-changing to see people who saw no future for themselves express long-term career and other life goals. The pride in the parents’ and guardians’ eyes is something I will never forget.”
The harsh reality of juvenile facilities is that many or maybe most of the teenagers in this room—who are all attending high school or college-level classes—wouldn’t have graduated from high school if they hadn’t been incarcerated. Maybe, Bennett says, they wouldn’t even have survived to adulthood (research shows a much higher morbidity rate for formerly incarcerated youth).
While some incarcerated youth may transition to adult prison after they turn 25, most will move back into their communities. The hope is that the health care they received—the dialectical behavior therapy (DBT) practices, the nutrition information, the personal hygiene tips, the ability to cope and flourish—will stay with them. Maybe it will even propel them to greater things; the College of Nursing has fielded several requests from formerly incarcerated youth now interested in a health care career.
At Decker Lake, Rutledge sends the graduates off with vaccine and dental records, along with any prescriptions they need for medications or glasses. She also adds some advice: Be careful of the crowds you hang around with. Be careful of the decisions you make. “I tell them they’ve been given a second chance, and to try not to end up here again.”
Then the graduates walk out the front door, finally free to leave the facility, to re-enter the world they left behind—even to visit the lake on the other side of the fence if they want. Wherever they go, they know a lot of people like Sandy Rutledge are cheering for them to succeed.
These ceremonies are a big deal at Decker Lake, including high school graduations each spring. “Their parents, guardians, case workers, and staff members all attend, and most of us are in tears,” says Danielle Bennett, a former psychiatric nurse student. “It’s life-changing to see people who saw no future for themselves express long-term career and other life goals. The pride in the parents’ and guardians’ eyes is something I will never forget.”
The harsh reality of juvenile facilities is that many or maybe most of the teenagers in this room—who are all attending high school or college-level classes—wouldn’t have graduated from high school if they hadn’t been incarcerated. Maybe, Bennett says, they wouldn’t even have survived to adulthood (research shows a much higher morbidity rate for formerly incarcerated youth).
While some incarcerated youth may transition to adult prison after they turn 25, most will move back into their communities. The hope is that the health care they received—the dialectical behavior therapy (DBT) practices, the nutrition information, the personal hygiene tips, the ability to cope and flourish—will stay with them. Maybe it will even propel them to greater things; the College of Nursing has fielded several requests from formerly incarcerated youth now interested in a health care career.
At Decker Lake, Rutledge sends the graduates off with vaccine and dental records, along with any prescriptions they need for medications or glasses. She also adds some advice: Be careful of the crowds you hang around with. Be careful of the decisions you make. “I tell them they’ve been given a second chance, and to try not to end up here again.”
Then the graduates walk out the front door, finally free to leave the facility, to re-enter the world they left behind—even to visit the lake on the other side of the fence if they want. Wherever they go, they know a lot of people like Sandy Rutledge are cheering for them to succeed.
![A youth walks out the door alongside unit supervisor [NAME] in the community room at Decker Lake Youth Center.](./assets/TmhVtlcmYV/door-overlays_edit_1-2451x1319.jpg)
![A youth walks out the door alongside unit supervisor [NAME] in the community room at Decker Lake Youth Center.](./assets/q9ol1PO6F6/door-overlays_edit_2-2451x1319.jpg)


First Steps to Redemption
March 27, 2026
Editorial Credits
Story by Elaine Jarvik
Photography by Laura Seitz
Design by Wesley Thomas
Research & Editorial Support by Lauren McKinnon
Art Direction by Jesse Colby
Editing & Publishing by Nick McGregor
For additional information, email jennifer.clifton@nurs.utah.edu